Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Just when the pandemic is spreading far beyond big cities, many rural hospitals are closing or set to close soon. Time reports:
Hospitals in St. Paul, Minn., Chicago, Houston and Philadelphia have recently closed or are set to do so soon. And in rural areas of the country, where hospitals often have enough beds for just a few dozen patients, 15 facilities have shuttered this year as of Oct. 20, including 11 since March, according to the Cecil G. Sheps Center for Health Services Research at the University of North Carolina at Chapel Hill. There may be as many as 18 such closures in 2020, topping last year’s record high. The hospitals in the worst financial shape generally have one thing in common: they serve the country’s most vulnerable people, who rely on Medicare and Medicaid or who are poor and uninsured.
When the pandemic struck, just about all hospitals took a financial hit. Cash-cow elective surgeries were suspended for weeks to curb viral spread. Hospitals that weren’t treating many COVID-19 patients simply ate that loss, while expenses skyrocketed at those that were, due to high demand for personal protective equipment and labor costs. A September report from hospital insights firm Kaufman Hall found that operating margins for U.S. hospitals were down 89% in the first eight months of the year, excluding federal relief funds.
Time reported that big city hospitals often have enough insured patients to make up for the money they lose when patients use Medicare or Medicaid. But in rural America, where some have no health insurance at all, hospitals can’t make it. One in five rural hospitals is at risk of closing and in some states — including Georgia — Time reports that up to 40% of rural hospitals are at risk of closing.

(Time)
The above chart shows what is happening year by year, but it does not tell the whole story.
Let’s put the figures on a different chart to see the cumulative effect.
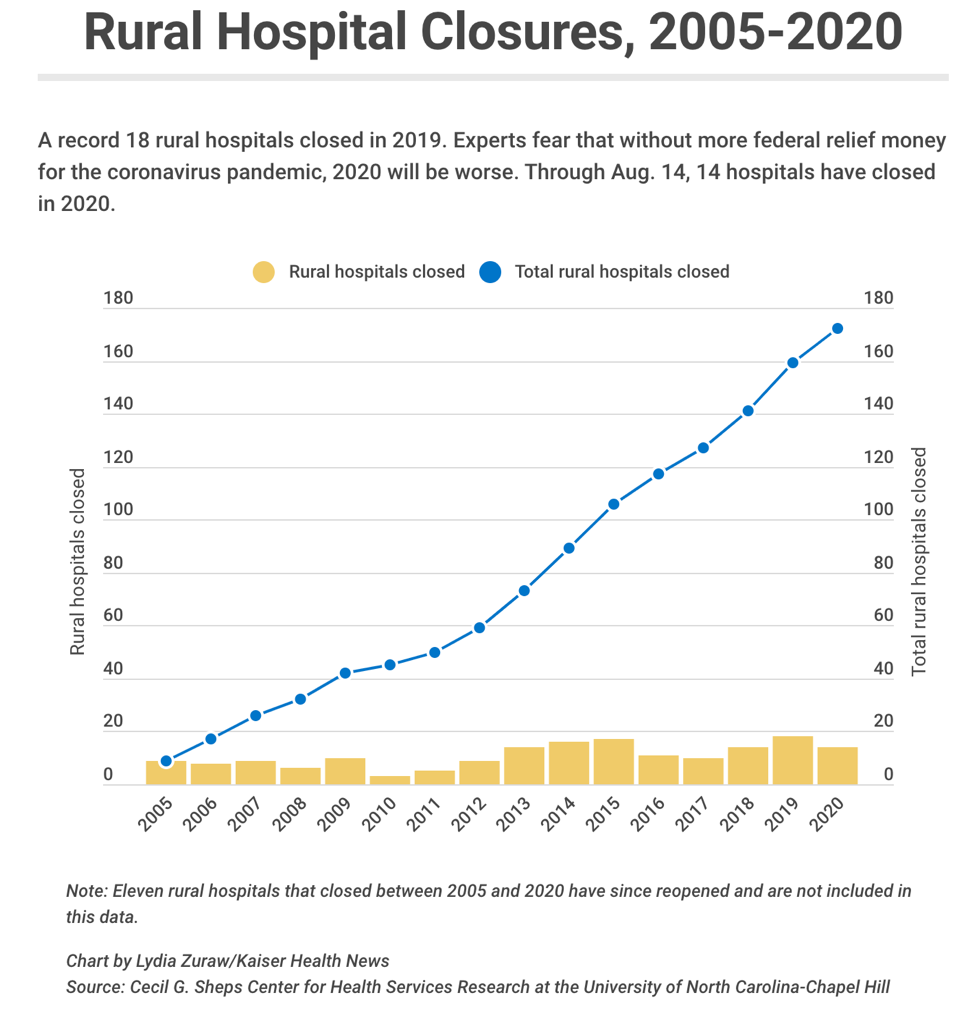
(Kaiser Health News)
Little by little, a dozen or two dozen annual hospital closings add up. The American Hospital Association estimates “57 million Americans depend on these hospitals. Beyond the health benefits, hospitals make a rural community economically attractive for both businesses and residents.”
Here is where 174 rural hospitals closed between 2005 and now.
As Time’s reporting says, the pandemic makes it far more likely that the pace of rural hospital closures will grow even faster.
A Kaiser Health News summary says:
Before the pandemic hit this year, hundreds of rural hospitals “were just trying to keep their doors open,” said Maggie Elehwany, vice president of government affairs with the National Rural Health Association. Then, an estimated 70% of their income stopped as patients avoided the emergency room, doctor’s appointments and elective surgeries.
“It was devastating,” Elehwany said.
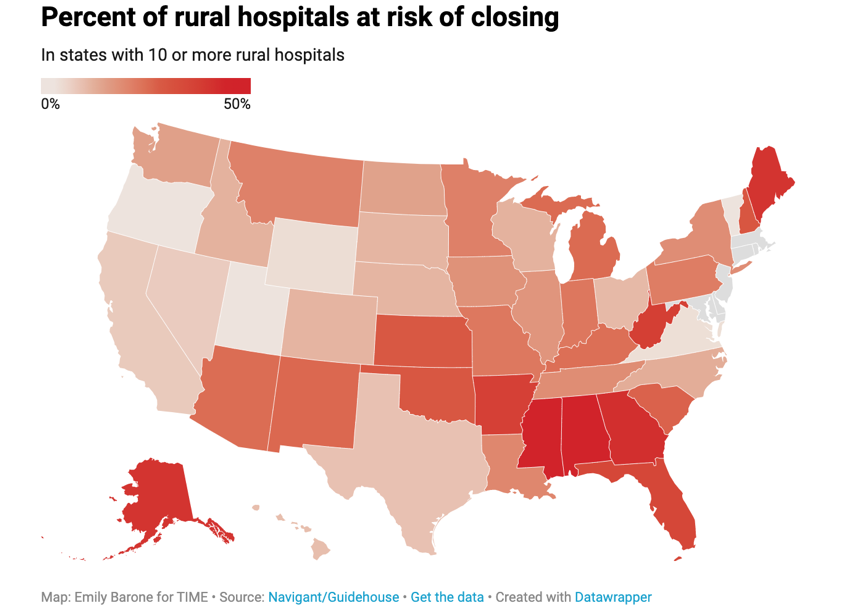
(Time)
Another challenge for rural hospitals, as Pew Research has found, is that rural communities — which have been losing population for a decade — may lose even more population during the pandemic. “With counties serving as critical providers of hospital and public health services,” Pew said, “the decline in the rural tax base has probably weakened the nation’s ability to respond to the crisis in many large, less populated areas.”
The National Bureau of Economic Research says when rural hospitals close, more people die from time-sensitive conditions. NBC News reported that when a rural hospital closes, death rates in the surrounding communities increase by nearly 6% — and that’s when there’s not a pandemic.
Earlier this year, the CARES Act sent $124 billion to health care providers, including physicians and medical clinics. Hospitals got about $70 billion of that. The American Hospital Association says it was not nearly enough:
U.S. hospitals and health systems will lose $120.5 billion between July and December 2020 due to reductions in patient volumes coming to baseline levels over the next 12 months. These losses are in addition to the $202.6 billion in financial impact the AHA estimated for hospitals between March and June 2020, bringing total losses for this calendar year to at least $323.1 billion, not including the impact of currently increasing COVID-19 case rates. If these surge trends continue, the financial impact on hospitals and health systems could be even more significant.

(Department of Health and Human Services)
Some small and mid-size cities are now cut off from air service

Some of the 88 American Airlines planes stored at Pittsburgh International Airport sit idle on a closed taxiway in Imperial, Pa., on Tuesday, March 31, 2020. (AP Photo/Gene J. Puskar)
As one who, in normal times, travels a lot to mid-size towns to teach, my future may involve a lot of driving. CNBC pointed to Dubuque, Iowa, as an example of a city “… where American Airlines suspended service in early October, (and) passengers will now have to drive three to four hours for a flight.”
American Airlines cut service to 15 U.S. cities. CNBC says:
Other airlines have made similar suspension decisions as the pandemic continues to put financial pressure on them. Delta Air Lines suspended service to 11 markets in July, and a spokesperson said it does not have a date to resume service, although it is monitoring demand. A United Airlines spokesperson said the carrier has added service to nine small communities, resumed service to six previously suspended and is continuing to evaluate the status of four others still suspended.
Business Insider produced a sample of cities that lost American’s air service starting this month and lasting for who knows how long:
- Del Rio, Texas (DRT)
- Dubuque, Iowa (DBQ)
- Florence, South Carolina (FLO)
- Greenville, North Carolina (PGV)
- Huntington, West Virginia (HTS)
- Joplin, Missouri (JLN)
- Kalamazoo/Battle Creek, Michigan (AZO)
- Lake Charles, Louisiana (LCH)
- New Haven, Connecticut (HVN)
- New Windsor, New York (SWF)
- Sioux City, Iowa (SUX)
- Springfield, Illinois (SPI)
- Williamsport, Pennsylvania (IPT)
Same-sex adoptions will appear before the Supreme Court soon
While you are rightfully focused on a Senate vote to confirm a new Supreme Court justice and on a pandemic and on an election a week away, you may want to be sure this is on your radar, too.
The day after the election, Nov. 4, the Supreme Court — including its newest justice — will hear a case that could have far-reaching implications for same-sex couples who want to adopt children. The case is styled “Fulton v. City of Philadelphia,” which was filed on behalf of Catholic Social Services.
On the surface, this might seem to be a narrow issue of a faith-based social services agency requesting to reject LGBTQ families and others whom they consider to be in violation of their religious beliefs. But legal scholars say it could have far broader applications.
Carlos Ball, a professor at Rutgers Law School, told NBC News:
“If the Supreme Court holds that religious organizations have a constitutional right to be exempted from anti-discrimination laws when they receive government money to conduct certain activities — such as placing foster care children with foster parents — that will significantly limit the impact and efficacy of civil rights laws,” Ball said. “It will essentially allow anyone who has a religious basis for discriminating to claim that they are constitutionally exempt from the application of civil rights laws.”
If the high court sides with Catholic Social Services, discrimination against LGBTQ people could “become part of the public child welfare system,” according to Leslie Cooper, deputy director of the American Civil Liberties Union’s LGBT and HIV Project.
“LGBT people would face discrimination in every state in the country, because many states partner with private agencies,” she explained.
Eleven states have laws on the books allowing for state-licensed agencies to claim religious exemptions in the foster and adoption process, and others are considering similar measures. Most recently, Tennessee Gov. Bill Lee signed a bill that permits adoption agencies to refuse to work with families if doing so would “violate the agency’s written religious or moral convictions or policies.”
The case began when the city of Philadelphia ended a contract with Catholic Services once the city learned the group would not consider same-sex couples as adoptive parents. The case has taken two years to wind its way to the Supreme Court after the court handed a victory to a Christian baker who refused to make a wedding cake for a gay couple.
Should people in prison be included in drug trials?
The New England Journal of Medicine includes an essay that examines the ethics of including people in jails and prisons in drug trials. It may not sound like much of a question until you consider the incredible abuse of this practice in the past. The Journal article says:
There are three arguments for enrolling incarcerated people in vaccine trials. First, it would offer them early access to a potentially efficacious vaccine. Second, it would provide them with a choice to participate in medical research that will be offered to nonincarcerated people. Third, it could shorten the amount of time needed to study vaccine efficacy, if transmission rates continue to be higher in correctional facilities than elsewhere.
Research involving incarcerated populations is ethically, legally, and logistically complex. Before the 1970s, it was common for incarcerated people to be disproportionately exposed to the risks and burdens associated with medical research. In response to research abuses, federal regulations classified incarcerated people as a vulnerable population for the purposes of medical research, making it difficult to conduct research in correctional facilities. More recently, there have been calls for the responsible inclusion of incarcerated populations in research as a means of expanding access to the potential benefits of participation.
But the argument goes that because prisons and jails have not shown themselves to be able to manage the pandemic, it may be too risky to include them in any drug trials. And then, ethicists worry that people who are incarcerated may feel they have no choice but to take part in the trials.
‘Physical distancing’ versus ‘social distancing’

Graduating seniors of a class of just over one hundred line up 10 at a time amid the coronavirus pandemic at Chattahoochee County High School on Friday, May 15, 2020 in Cusseta, Ga. (AP Photo/Brynn Anderson)
I have the BEST readers for this column and one of you, Deborah Lynn Blumberg, dropped me a note to suggest a different way of talking about how we need to physically distance from each other. Deborah writes:
I was speaking with a psychologist today for a story I’m working on. I can’t remember, but have you discussed the distinction between social distancing and physical distancing? I still see so many news stories talk about “social distancing” while psychologists I talk to in my reporting keep stressing that we should be saying “physical distancing” instead because we shouldn’t be socially distant from people right now since that’s a negative for our mental health — we need to connect with other people in safe ways. This could be something good for journalists to think about/remember as they’re writing, especially as we get into winter months and many people grapple with SAD, which therapists believe will be worse for people this year.
Deborah is exactly right. Social distancing can, according to researchers, even have a physical impact on people, particularly seniors.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.