Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
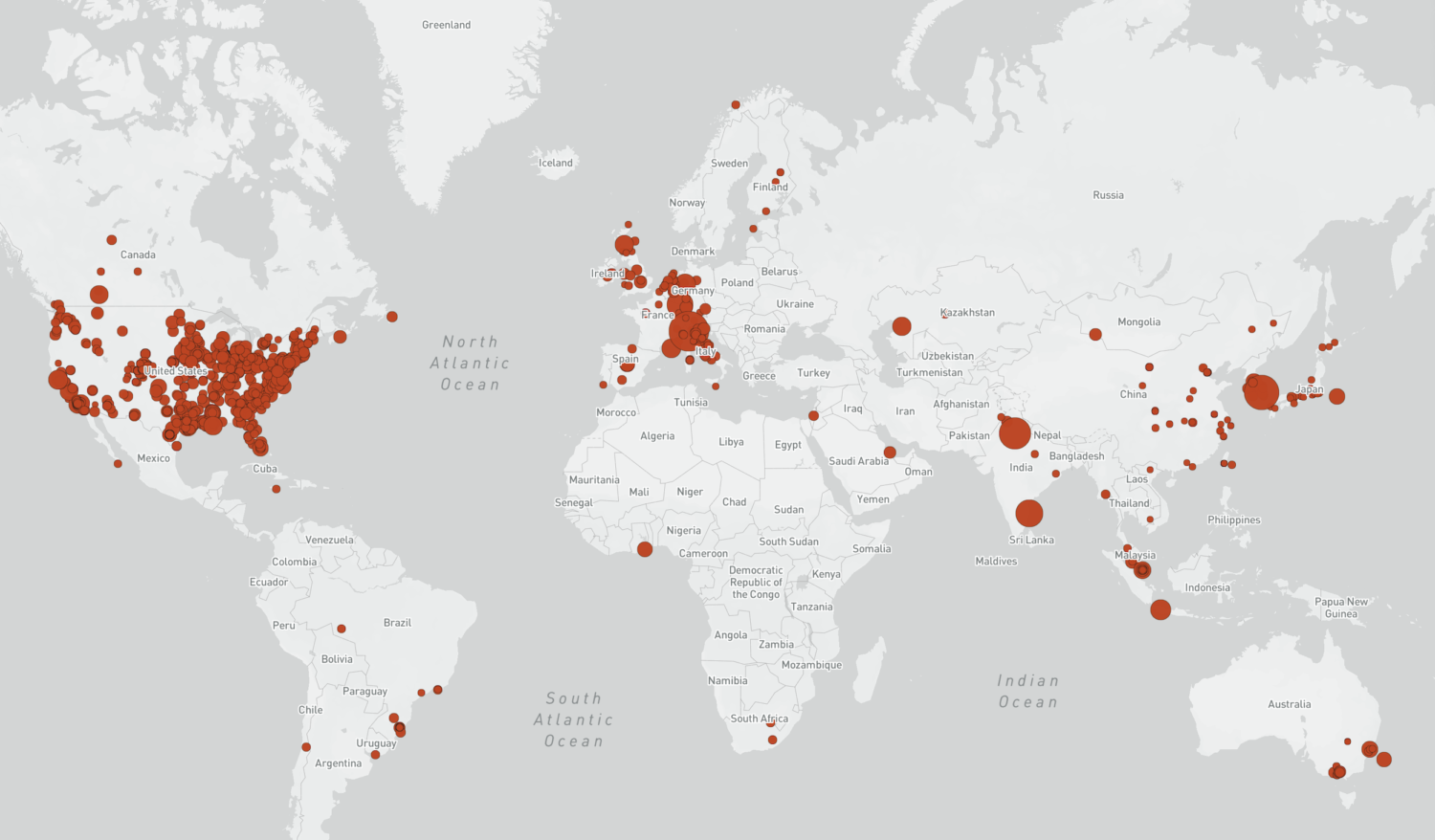
Professors and Ph.D. students at the London School of Hygiene & Tropical Medicine have pulled together an incredibly useful database of known superspreader events from around the world. It pulls together four existing databases into one.
The database describes where the event happened, what kind of location it was (such as a prison, meat processing plant, nursing home, etc.) and, interestingly, provides the geographic coordinates that make it easy to map. Look at the U.S. data and you will be overwhelmed by the number of these superspreader events that were in prisons, a few weddings and nursing homes.
This is exactly the kind of geeky thing that journalists will download, sort, map and chart. If you don’t know how, start here, or just define the data and drop it in here and it will map it for you. You are going to look like a genius.
You can look at and use this data in three ways:
Google sheet: view the database; download or make a copy to edit and sort
Bubble map: shows all the superspreading events in the database on a world map; click on a bubble to find more information about an event
Bubble map with timeline: same but with an animated timeline showing the events as they occurred in time
These superspreader events are important, as Vox explains:
Early contact tracing studies suggest these events have been a large driver of transmission around the world. By some estimates, 10% of people have been causing 80% of new infections.
This is one of the reasons experts worry about large indoor gatherings — more so than outdoor ones — causing large spikes in case numbers.
Kristin Nelson, an assistant professor of epidemiology at Emory University Rollins School of Public Health, joins a series of researchers who are publishing their findings about superspreader events. Smithsonian Magazine reported:
(Nelson’s) paper, a preprint accepted for publication, found that 2% of people were responsible for 20% of transmission. Other studies also have uncovered a similarly strong correlation between small numbers of people and wildfire viral spread. Researchers examining outbreaks in Hong Kong found that 20% of people created 80% of transmissions while about 70% did not infect anyone. In Israel, investigators looking at 212 cases concluded that they could be linked back to 1 to 10% of people. In a peer-reviewed paper, Adam Kucharski, an associate professor at the London School of Hygiene and Tropical Medicine, has estimated that 10% of people may be responsible for 80% of the cases.
The Washington Post explored one such event in Michigan where 187 people were infected at a local restaurant/pub. Smithsonian Magazine explained that one reason COVID-19 is so difficult to combat is because it is most contagious before symptoms appear, so people are spreading the virus without knowing it.
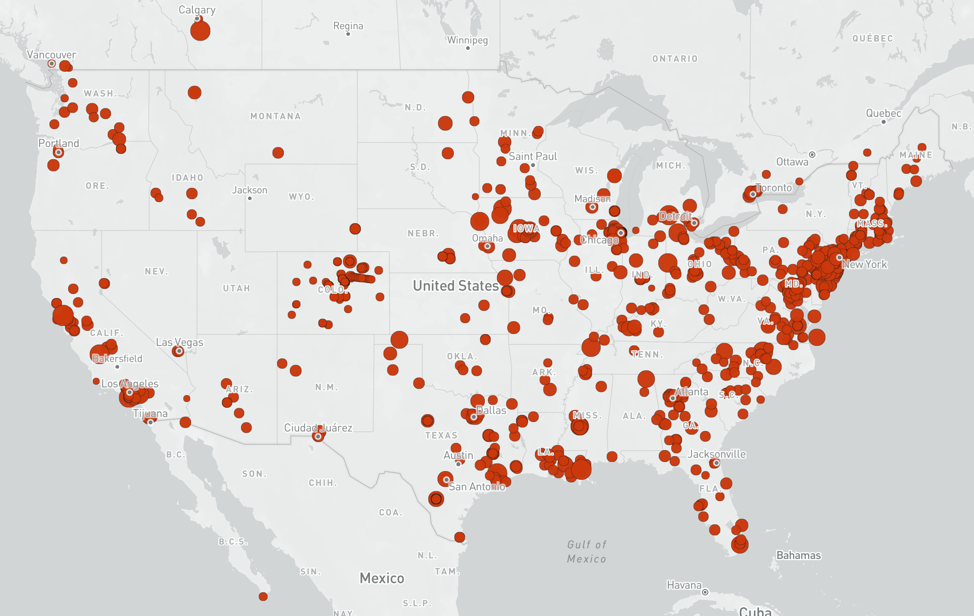
You can click on the interactive map and see the data behind each location. (London School of Hygiene & Tropical Medicine)
Isolation and quarantine are not the same
My friend Dr. Mona Khanna dropped me a note to say the words “isolation” and “quarantine” have different and specific meanings in the medical world. Maybe you knew this. I didn’t.
“Isolation” separates sick people with a contagious disease from people who are not sick.
“Quarantine” separates and restricts the movement of people who were exposed to a contagious disease to see if they become sick.
So, all of us who said the president and first lady were in quarantine had it wrong. They were quarantined while they awaited the test results. Then they isolated.
So, as Dr. Khanna emphasizes, “When someone is diagnosed with COVID-19, he/she is ‘isolated.’ When someone is exposed to a person with COVID-19, he/she is ‘quarantined.’ Once he/she turns positive, that becomes ‘isolation.’”
“If you included these definitions in your next column about COVID-19,” she says, “I betcha lots of reporters would start reporting it right!”
Only 3% of people who signed up for COVID-19 vaccine trials are Black
Drug companies are having a lot of trouble recruiting Black Americans to participate in COVID-19 vaccine trials. So far only 3% of the volunteers are Black. That is a problem for researchers who need to test the vaccine across a wide range of demographics to make sure vaccines are safe and effective.
The New York Times reported that with mistrust of vaccines at such a high level, researchers are going into neighborhoods seeking volunteers:
“Historically, we test everything in white men,” said Dr. (Nelson L.) Michael, a member of the vaccine development team at Operation Warp Speed, the public-private partnership set up by the White House. “But the disease is coming after people of color, and we need to encourage them to volunteer because they have the highest burden of disease.”
Now, academic researchers at trial sites like Pittsburgh’s are turning to neighborhood leaders to attract more diverse pools of participants. The Urban League of Greater Pittsburgh sponsored an information webinar and the New Pittsburgh Courier, which has a large, African-American readership, published articles about the trial.
While Black people stand to benefit greatly from a coronavirus vaccine, surveys show that they are the group least likely to trust one. In a poll last month by the Pew Research Group, only 32% of Black respondents said they were likely to take it, compared with 52% of white respondents. Historically, Black people have been more hesitant than other groups to get vaccines, especially the flu shot, and are also far less likely to volunteer for medical research; one study showed their participation hovering at about 5%. They are 13% of the population.
Black Americans have historical reasons to distrust drug trials. A short list would include:
…surgeries by Dr. J. Marion Sims, a 19th-century gynecologist, on enslaved Black women, the 40-year-long Tuskegee study, in which doctors deliberately allowed syphilis to progress in Black Alabama sharecroppers, and researchers’ taking of cells without permission from Henrietta Lacks, an African-American cancer patient, in 1951.
SPONSORED POST:
A Trint Webinar: Join Trint’s CEO & Founder Jeff Kofman (Emmy award-winning reporter and correspondent) and a panel of experts to learn how tech can enable journalists during the 2020 election. Join us at noon (EST) on October 13.
The government is starting to forgive PPP loans this week
Even while Washington is tied up in knots over whether it can find a way to agree to an economic stimulus plan, the Small Business Administration has begun formally forgiving the Payroll Protection Plan “loans” that it doled out earlier this year.
In order to earn forgiveness, businesses had to comply with a number of criteria, including that they would maintain their staff or quickly rehire those who were furloughed. And the businesses have to show that they used at least 60% of their loan for payroll expenses. The rest could be used for everything from rent to utilities, but the point of the program was to keep employees on the payroll.
96,000 of those loans went to restaurants.
This would be a good time to go back to those businesses that you spoke with in the early days of the pandemic to see if they got the loan forgiveness they counted on and what they say now about the need for Congress and the president to find some common ground on a new stimulus.
Governor tells diners to wear masks between bites
California Gov. Gavin Newsom tweeted:
Going out to eat with members of your household this weekend? Don’t forget to keep your mask on in between bites.
Do your part to keep those around you healthy. #SlowtheSpreadhttps://t.co/snYe5v55Rw pic.twitter.com/Y4fcDO5Zke
— Office of the Governor of California (@CAgovernor) October 3, 2020
Twitter did not respond kindly to the notion of remasking between bites. Some pointed out that the World Health Organization’s guidelines tell us not to touch our masks if we can help it, which would suggest not to keep putting your mask on and taking it off every time you take a bite. Nothing is easy in 2020.
COVID-19 can live on the skin for 9 hours
It seems like every day we learn something new about this virus. New research shows the coronavirus can live on human skin four times longer than the seasonal flu virus. The result of this finding is, no surprise here, to wash your hands.
LiveScience reports, “Earlier in the pandemic, researchers in the U.S. analyzed how long SARS-CoV-2 could last on surfaces and found it remained viable on copper surfaces for up to 4 hours, on cardboard for up to 24 hours and on plastic and stainless steel for up to 72 hours.”
COVID-19 reinfections are sometimes worse
There is not a ton of data on this yet, but researchers are paying attention to COVID-19 patients who are becoming reinfected. The second time around can be worse than the first bout with the virus.
The first reinfection case showed up in Europe in August. That one was asymptomatic. Researchers had hope that might be the norm for reinfections. But as reinfection cases piled up, in Hong Kong; then Reno, Nevada; then the Netherlands; Ecuador and India; some of the reinfections have been worse than the first round.
In India, for example, doctors say nurses were reinfected and that the second cases were worse partly because the patients had not fully recovered from the first illness.
“It’s really hard to find a pattern right now,” said Akiko Iwasaki, a professor of immunobiology at Yale University who has been following cases of reinfection closely. “Essentially every case is different.”
The difficulty in studying these second-round cases is that doctors have to look at the genetics of the first case versus the second one to know they are in fact separate viruses.
The good news is that it still appears that most people who are COVID-19 infected have what Danny Altmann, professor of immunology at Imperial College in London calls 90% protection “for a while.” But it is too early to know what “a while” means, whether it is months or longer or less.
Masks are required at many polling places

Pat DeVito cleans a voting booth during early voting at the Cuyahoga County Board of Elections, Tuesday, Oct. 6, 2020, in Cleveland. (AP Photo/Tony Dejak)
At least 33 states now say they will require voters to wear masks at the polls. Some states are going to offer curbside voting for people without masks.
ABC News points out that while retailers can turn people away for not wearing masks, the legality of turning people away from polls for not wearing a mask may be dubious. ABC says:
None of the states reached out to by ABC News said they are prepared to turn away voters who refuse to wear masks, but many said they are making preparations, like trying to head off crowds by encouraging people to use mail-in ballots and or allowing curbside voting and special booths where workers can wear protective equipment.
New York election officials will require voters and poll workers to wear masks at the polls, but they will also recommend that each polling site have an isolated area where poll workers in protective equipment can assist voters who are unable or unwilling to wear masks.
Voters who do go to the polls can expect a very different experience than normal. You may see plexiglass barriers separating voters and poll observers and lines may be longer because of spacing requirements.
Did your state overpay unemployment benefits? They are coming to collect from hundreds of thousands
The list of states that are just discovering that they overpaid unemployment benefits is growing. Already, North Carolina, North Dakota, Ohio and Texas say they are going to be asking hundreds of thousands of people for some of the money back. Some are already withholding parts of future payments.
In Texas alone, more than 185,000 people will be paying back some of the $203 million the state overpaid. In Pennsylvania, the state mistakenly sent duplicate payments to 30,000 people.
Open the windows: another simple COVID-19 prevention

A man pets a dog that sits in a window downtown Prague, Czech Republic, Tuesday, March 24, 2020. (AP Photo/Petr David Josek)
This simple solution may be especially important after the Centers for Disease Control and Prevention updated its guidance this week to say the virus can also be “airborne,” meaning it can linger in the air for minutes and maybe longer.
An easy way to fight the spread of COVID-19: Open the windows. The Duluth News Tribune looked back 100 years and found that during the 1918 pandemic, there was great debate over whether streetcar windows should be open. The story says:
The Minneapolis health commissioner decided “streetcar windows will be kept open until the temperature drops to the freezing point, when they will be closed if the car is heated and a ventilation system is installed.”
At one point during that pandemic, experts recommended giving children extra credit in school if the slept with the windows open.
And, the story adds:
This week, the German Chancellor Angela Merkel promoted the opening of windows on the hour as “one of the cheapest and most effective ways” of containing the virus. Germans already were used to the practice of opening windows once in the morning and once at night. Now schools in that nation are being asked by official health guidance papers to bring in a draft for three to five minutes, every 15 to 20 minutes.
The Guardian points out that in winter, we will close windows and trap air inside, leaving it uncirculated.
Since it has become known that 90% of COVID-19 patients pick up the virus indoors, the practice has come into its own. With winter on the doorstep, it will become even more important, experts insist.
Even without coronavirus, Martin Kriegel, an engineer and air current analyst at the Technical University in Berlin, told Die Zeit, “there is clear evidence that air quality in offices correlates with the number of days workers are off sick”.
Schools, which have increasingly been viewed as a testing ground for how society can learn to live with the disease, have long since adopted the practice. A recent gathering of the ministers of education for Germany’s 16 states was dedicated to how to air a classroom. Five experts, from fluid mechanics to indoor air hygienists and aerodynamicists, reinforced the importance of airing a room every 15 to 20 minutes, for five minutes in spring and autumn, and three minutes in winter.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.
Al Tompkins is senior faculty at Poynter. He can be reached at atompkins@poynter.org or on Twitter, @atompkins.