Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
A week ago, Centers for Disease Control and Prevention director Robert Redfield was being painted in media as being under President Donald Trump’s thumb. On Tuesday, he broke into an open field running.
During a livestreamed interview, Redfield told Dr. Howard Bauchner, editor of the Journal of the American Medical Association, “I am worried. I do think the fall and the winter of 2020 and 2021 are probably going to be one of the most difficult times that we have experienced in American public health because … of the co-occurrence of COVID and influenza.” (Go to 19:06 to hear this quote.)
Redfield said that it is time to get serious about the universal use of face masks. He said if everyone in the country wore masks in public it would bring the spread of the coronavirus under control within four to eight weeks.
“The time is now. The data is clearly there. Masking works,” Redfield said. He went on to say the president and vice president need to “set an example.”
Also Tuesday, Redfield co-authored a JAMA essay pointing out that masks slow the spread of COVID-19, and that even homemade masks help. The essay said:
The public needs consistent, clear, and appealing messaging that normalizes community masking. At this critical juncture when COVID-19 is resurging, broad adoption of cloth face coverings is a civic duty, a small sacrifice reliant on a highly effective low-tech solution that can help turn the tide favorably in national and global efforts against COVID-19.
The CDC published a study focused on a hair salon in Springfield, Missouri. Two stylists there were symptomatic COVID-19 patients who, while infected, came into contact with a combined 139 clients. But, the study said, the stylists wore masks — and no symptomatic cases resulted from that exposure.
When will there be a vaccine? Best case, months away, probably longer
Redfield said in the interview with JAMA that he is “very optimistic” about the prospects of a vaccine.
“The mission is to have a vaccine available to the American public by January 2021,” he said. He also said, “I am optimistic we will have one or more vaccines available by the first of the year.”
My colleagues at PolitiFact have been tracking this question based on where drug trials stand and how they are progressing and not on the hopes of politicians. The best estimate now is if all goes well, the earliest we could have a COVID-19 vaccine is late spring 2021.
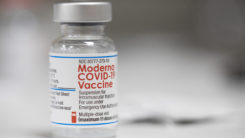
We learned Tuesday that Moderna, which for a while was thought to be the leading developer of a vaccine, is about to enter phase 3 trials on July 27. Moderna, which has gotten a lot of publicity, jumped back in the news again announcing that it had tested a two-shot vaccine on 45 people ages 18 to 55. The test involved three dosages from low to high. The highest dose produced the most antibodies but also caused fatigue, chills, headaches, myalgia and pain at the injection site for several of the subjects.
In the phase 3 trial, which includes 30,000 Americans, we will find out if the vaccine actually works. To this point, we don’t have any evidence that it is effective in preventing COVID-19.
My colleague Louis Jacobson reported that two other possible vaccines are in phase 3 clinical trials. Once those trials are completed, they would be candidates for approval. Keep in mind that most drugs that enter phase 3 trials do not make it to production because they cannot be proven to be safe and effective.
Jacobson reported, “Another eight vaccines have begun phase 2 trials. And more than 100 other vaccines that haven’t begun clinical trials are in the pipeline.”
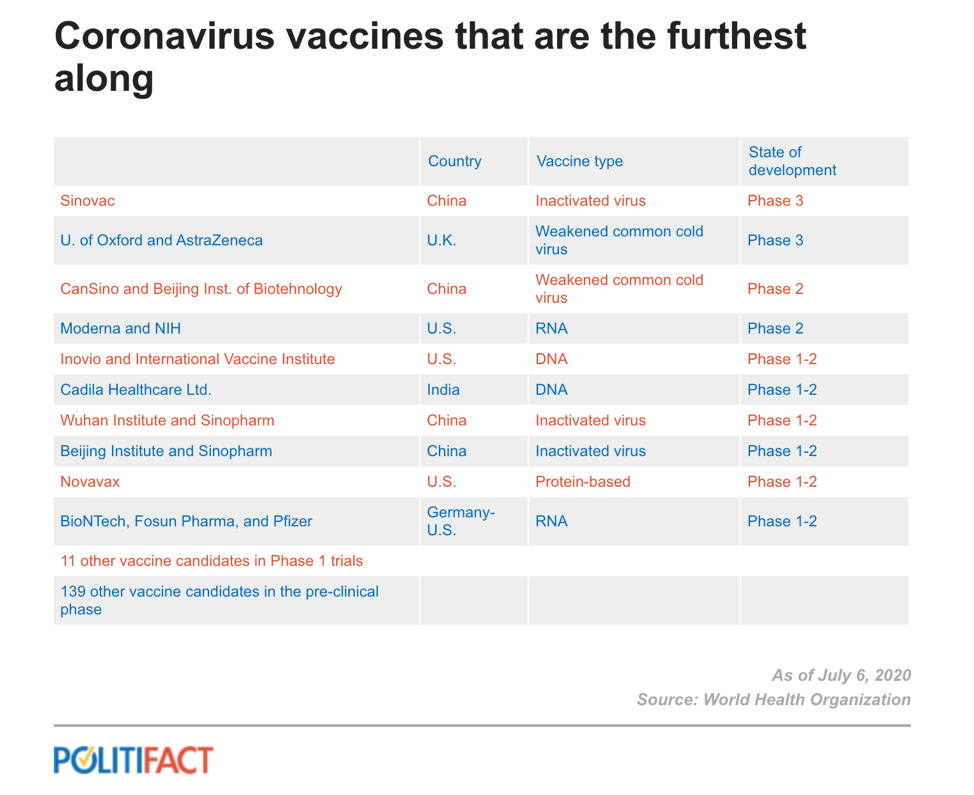

(Data from WHO, graphic from PolitiFact)
This is actually fast progress compared to how long it usually takes a vaccine to make it to market. Think about the implications of not having a vaccine until late spring. What would that mean for schools trying to think through how long they might be teaching virtually? What would it mean to the future of business and manufacturing? How will the threat of a looming pandemic affect our mental health if it lasts for more than a year?
Get local: There are 2,956 clinical trials underway in the United States related to COVID-19. They are underway in every state and you can look them up right here. The U.S. National Library of Medicine’s clinical trials site tells you what is being researched and who is doing the work.
Parents are struggling with back-to-school decisions
With the CDC director’s sobering concerns and the prospect of no vaccine until late spring at the earliest, the difficult decisions ahead seem to be getting real for parents. In a matter of weeks, they will have to send kids back to school, keep them home to home-school or learn to live with a hybrid system of sending them to school some days and keeping them home other days.
South Carolina’s governor announced Tuesday that his state’s schools would open Aug. 17, but some students will only attend in-person classes every other day or every other week.
This week, Los Angeles and San Diego schools decided they would be online for the fall. Those decisions affect 825,000 students. San Diego schools, until recently, planned to reopen for five days a week. But when they calculated the costs of constant cleaning, delivering food to classrooms and changing bus schedules, they found it would cost about $50 million more than the current budget.
The American Federation of Teachers, a union that represents teachers, said the national cost for running schools safely would be about $116 billion over current spending. The Council of Chief State School Officers pegged the tab even higher, between $158.1 billion and $244.6 billion.
Whatever the cost, the decision to reopen or to remain virtual may not be a matter of what educators think kids need to learn best, but instead a matter of money. Schools are discovering that they don’t have the money they need to reopen and come anywhere close to the safety guidelines that the CDC recommends and that teachers and parents demand.
Why does reopening cost so much? The Association of School Business Officials calculated the needs of “an average school district with 3,659 students, eight school buildings, 183 classrooms, 329 staff members, and 40 school buses (transporting at 25% capacity, or 915 students, to comply with recommended social distancing guidelines).” That is about the size of the average district in several states:
Here’s what they found:

(From the Association of School Business Officials International)
Omaha, Seattle and other cities are working on plans that would bring students in a couple of times a week: half on Tuesdays and Thursdays, half on Mondays and Fridays, with Wednesdays being rotated between the groups. There are various iterations of the schedule, but they all have one thing in common: The fall semester will not look like any that came before it.
Take just one sliver of the challenge as an example of the complexities school systems face: busing. The CDC’s guidelines suggest not delivering students all at the same time, but to stagger pickups and deliveries, meaning buses would have to make multiple runs.
That would jack up fuel costs and maintenance costs as buses travel more miles. It might require more drivers and more buses or additional costs to clean and sanitize buses. EdWeek pointed out:
Guidance from the Centers for Disease Control and Prevention recommends six-foot distancing on school buses. Adhering to those guidelines would drastically reduce the seating capacity of most buses; a large school bus can sit between 50 and 72 students. To fit more students on buses, districts could allow siblings to share seats and find other ways to tweak the CDC guidance, but likely will not be able to solve the problem altogether. For the foreseeable future, schools will no longer be packing two or three students in each bus seat.
Would teachers return if schools reopened?
About one in four teachers are considered “at-risk” if they return to classrooms. President Trump suggested that older or health-compromised teachers could “sit it out for a little while,” until there is a vaccine. Two polls, one by EdWeek and the other USA Today/Ipsos, show that somewhere between 10 to 20% of educators would quit or are considering quitting if they are told to go back in the classroom while the pandemic is still spreading.

(From the Kaiser Family Foundation)

(From the American Enterprise Institute)
The American Enterprise Institute suggested:
When discussing reopening plans for the 2020–21 academic year, schools should consider measures such as providing early retirement incentives and creating new roles for teachers and principals who are forced to remain at home due to their risk. Additional policies will be needed to give schools access to teachers who can backfill these positions.
The AEI expanded on that idea and said retired teachers could be great for helping students catch up:
Teachers sheltering in place could provide online instruction, remote tutoring, online mentoring, or televised instruction with the right professional development and support. For example, the British government launched the Oak National Academy using 40 teachers who provide more than 180 hours of lessons each week. States and districts have launched partnerships with local public media to provide televised instruction with local teachers.
Platforms such as Outschool, Weekdays, BetterLesson, and Tutor.com offer opportunities for teachers to serve students in online classes and tutoring sessions. Note that teachers of all ages may be interested in these options.
AEI recommended that “state policymakers and school districts could revisit teacher certification requirements and reciprocity agreements to make it easier for a teacher certified in one state to teach in another. States are considering similar provisions to help surge health care capacity to overwhelmed hospitals.”
And maybe universities could work with school districts to pair soon-to-graduate teachers with those who are sheltered at home.
What have other countries done?
President Trump pointed to other countries that successfully reopened schools as evidence that the U.S. can do the same. MIT researchers wrote that those countries are different from the U.S. in two key ways:
Schools have had to close in 191 countries, affecting more than 1.5 billion students and 63 million teachers, according to the United Nations. But in many countries, schools are now cautiously reopening: in Germany, Denmark, Vietnam, New Zealand, and China, children are mostly back behind their desks. These countries all have two things in common: low levels of infection and a reasonably firm ability to trace outbreaks.
How vulnerable are children if they do go back to class?
Children are about half as likely as adults to be infected with COVID-19. But children tend to get closer to each other than adults do, which increases the likelihood that a child in school could be infected.
Children who do catch COVID-19 usually get mild effects. About one in five patients ages 10-19 have any clinical symptoms, compared to about 69% of adults.
The MIT research said:
A preprint in the journal Public Health found that across seven countries up to May 19, there were 44 COVID-19 deaths out of over 137 million children 19 and under. That’s a rate of less than 1 in 3 million. There is an unpleasant new COVID-linked inflammatory syndrome in children similar to Kawasaki disease, but it’s extremely rare. “I think there have been fewer than 500 cases reported worldwide,” says Tina Hartert, a medicine professor at the Vanderbilt Institute for Infection, Immunology, and Inflammation in Nashville, Tennessee. The message seems to be that parents should not worry unduly about what might happen to their kids should they catch the virus.
But another question is to what extent children may spread the virus. At this point, we just don’t know for sure. Two studies, one from France and one from Germany, had different findings about to what extent children spread the virus to adults. Another study from China found that children bring COVID-19 home from school.
The National Institutes of Health is currently using nasal swabs to study 2,000 families in 10 cities every two weeks. The lead researcher is Tina Hartert, a Vanderbilt University medical professor.
The Trump administration backed down, international students can stay
Just as eight universities were hauling the Trump administration to court over the U.S. Immigration and Customs Enforcement’s decision that international students would have to transfer to a new school or go home if their classes were all online, the government backed down. The threat sparked protests from hundreds of schools that are still refining plans on how or even whether to reopen campuses in a matter of weeks.
About a million international students attend college classes in the U.S. each year, which accounts for nearly 5% of all students enrolled in colleges and universities in America.
Universities were desperate to keep international students enrolled because, usually, they pay a much higher tuition than American students pay.
Get local: Here is data about how many international students attend U.S. schools, which schools have the biggest international student population and what international students study.
New guidelines are out on what we should eat
Today, the Dietary Guidelines Advisory Committee will issue its final recommendations to the government for healthy eating. The committee is advisory and does not write the rules.
Two of the more controversial recommendations involve alcohol and sugar.
The guidelines will lower the recommended limit of alcoholic drinks per day for men to one. The current recommendation is for men to limit their intake to two drinks per day and one drink per day for women.
Even while we are snacking our way through the pandemic, the committee will recommend that we all cut down on added sugars. And the committee will take aim at sugars for children under 2 years old, suggesting an outright ban on giving little children sugar-sweetened beverages. For babies, the recommendation includes small amounts of food starting at 6 months of age, and dairy products are part of that list.
The Center for Science in the Public Interest said:
We welcome the committee’s strong recommendation to reduce Americans’ consumption of added sugars from less than 10% of calories to less than 6% of calories for anyone aged 2 or older. Although a separate subcommittee failed to reach a strong conclusion on the impact of sugary drinks on weight gain (based on a review of evidence from 2012 to 2019), the overall stronger limit on added sugars, which is based on a broader body of evidence, is an indication that a healthy diet leaves little room for excess sugars, including from soda and other sugary drinks.
Members of the committee are largely university-based so you may find somebody on the list near you.
The guidelines are important for a lot of reasons:
- They are the basis for the U.S. Department of Agriculture’s School Lunch Program and School Breakfast Program.
- They made up what you may know as “the food pyramid.”
- Today, about half of all American adults have one or more preventable, chronic diseases, many of which are related to poor quality eating patterns and physical inactivity. Rates of these chronic, diet-related diseases continue to rise, and they come not only with increased health risks, but also at high costs.
The beef industry said the guidelines are too tough on meat consumption, while the dairy industry is happy that the guidelines stick with the old recommendations of three servings of dairy products a day.
Early in the process, the Trump administration limited the scope that the committee would consider, including meat consumption guidelines. These are the 80 questions the committee did consider.
The key here is that this is the ninth edition of these guidelines and we just keep getting fatter and more unhealthy with each passing edition.
One question produced a study that found Americans eat, on average, 5.7 times per day and 93% of us are snackers. Snacks encompass about a fourth of our caloric intake on any given day.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.
Al Tompkins is senior faculty at Poynter. He can be reached at atompkins@poynter.org or on Twitter, @atompkins.