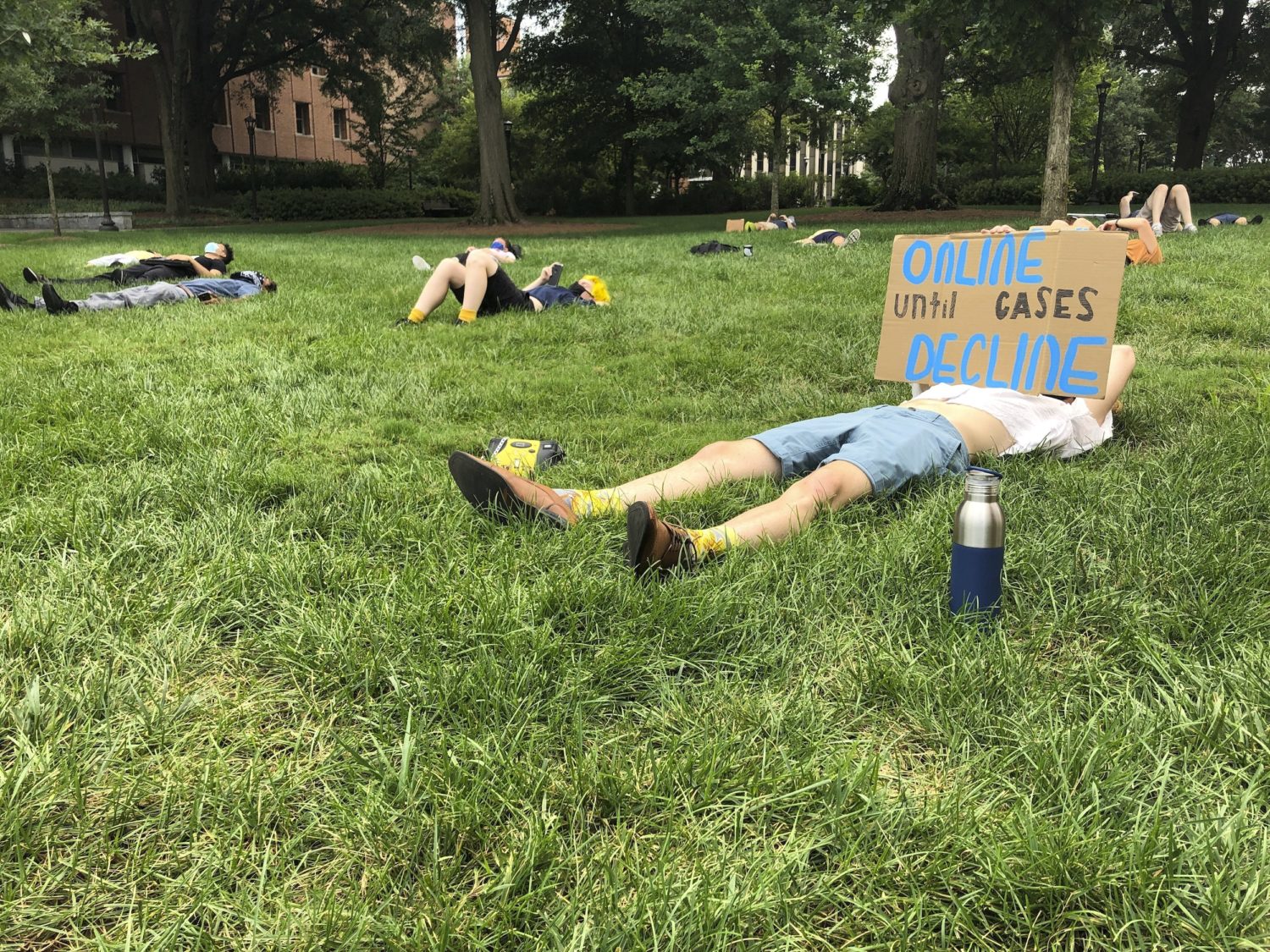Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
We are barely a week into the fall semester and the outbreaks have begun.
The University of North Carolina announced Monday that it is suspending in-person classes.
Barbara Rimer, dean of UNC’s Gillings School of Global Public Health, said in a blog post Monday that universities have to keep an eye on financial concerns, but that finances cannot be the deciding factor for closing campuses. The grim assessment one week into the semester may forewarn what is ahead for other schools:
Carolina Together, the plan for how the university would return to on-campus operations, indicates that if certain conditions prevail, it might be necessary to take an off-ramp and return to remote operations for teaching and learning. Most likely, that also would result in reductions in students living in dorms.
The rationale for taking an off-ramp now is that the number of clusters is growing and soon could become out of control, threatening the health of others on campus and in the community and putting scarce resources at risk. While it appeared that students on campus were compliant with distancing and mask use, reports of off-campus behavior showed a different pattern — drinking, no masks or distancing, and crowds. I do not have first-hand observations; this generalization reflects what has been reported and reflected in increases in numbers of cases, reflecting mostly dorm and fraternity-based clusters.
After only one week of campus operations, with growing numbers of clusters and insufficient control over the off-campus behavior of students (and others), it is time for an off-ramp. We have tried to make this work, but it is not working.
The school sent an email to students that said they could cancel housing contracts with the school without penalty and that students who had no other place to go could stay on campus.
The last few days set the stage for what unfolded at UNC.
UNC’s Sigma Nu fraternity house was named a COVID-19 cluster, which means health authorities identified five or more cases in that location. The fraternity house is now quarantined.
But it did not stop there. An alert Sunday told students about a COVID-19 cluster in a residence hall.
!Alert Carolina! Emergency Notification: Cluster of COVID-19 cases at Hinton James. https://t.co/qPgkjGbvvI
— Alert Carolina (@AlertCarolina) August 16, 2020
The Daily Tar Heel reported that there have been four COVID-19 clusters at UNC in the last three days.
UNC is hardly alone in facing the harsh realities of reopening.
NBC News said 23 people who are members of a sorority chapter tested positive at Oklahoma State University. The school put the entire sorority house under quarantine.
Meanwhile, at Colorado College, one student’s positive diagnosis prompted an entire 155-person residence hall to be quarantined for 14 days. The Colorado Springs Independent reported that the infected student tested positive before arriving on campus and then did not social distance, so others were at risk. The acting dean of students didn’t seem pleased in a note to students when reminding them they were supposed to have stayed away from others while they awaited their test results.
Notre Dame started the week off with disturbing news. The South Bend Tribune reported:
On Friday alone, the university reported 10 new cases. Of the 348 tests, 160 were performed on students and staff members with the football program. Many of the other tests were conducted on students who were either symptomatic or potentially had contact with symptomatic students.
And the numbers grew only worse over the weekend. Saturday, three of 11 tests came back positive, for a 27.3% positive rate. Sunday saw 15 new infections out of only 30 tests.
More than a quarter of Notre Dame’s 58 confirmed cases since Aug. 3 came on Sunday, with its 50% positive rate.
And hundreds of Northeast Mississippi Community College students are quarantined because of nine positive COVID-19 cases there in the last two weeks. That quarantine involves fully one out of 10 students enrolled there, plus another two dozen of the school’s staff.
The school’s president said, “We’ve had students that are on quarantine that have come to class and said, ‘Well I didn’t think I was quarantined from all my classes, just that one class.’”
The school of 3,034 students set aside 18 dorm rooms for quarantined students to use. It has not filled them up yet, but plans to keep rotating students through the rooms as the pandemic rolls on.
And in an unfortunate case of bad timing, Boston University said there is no connection between the pandemic and its recent announcement that updated how it would award posthumous degrees to students who die before graduating.
Colleges are tacking on COVID-19 fees
This won’t go over well. College students were already complaining about paying fees for services that they won’t get to use this semester. Now they are facing COVID-19 fees as high as $450 to cover testing and cleaning and other expenses that schools are incurring.
The University of Michigan is charging $50. Merrimack College in Massachusetts plans to charge $450. The New York Times surveyed schools around the country and found:
Baylor University said it was sending home test kits to all students, and is requiring negative results before students arrive on the campus in Waco, Texas. The school will also conduct testing throughout the semester. Baylor is covering the costs, a spokeswoman said.
Elon University, a private institution in North Carolina with about 6,300 undergraduates, is also sending home testing kits to incoming students. The university will charge students $129 but is giving them time to seek reimbursement from their health insurer or apply for a fee waiver before billing them. Students can seek tests elsewhere, at a lower cost, as long as the test meets Elon’s requirements. Random testing will occur throughout the fall, at the university’s expense.
The Times story said a student’s health insurance may reimburse for COVID-19 testing expenses if the test is “medically necessary,” meaning the student would have to show symptoms or have been notified that they were exposed to someone who tested positive.
COVID-19 testing protocols for more than 500 universities
A couple of researchers at CalTech have pulled together a remarkable list of COVID-19 testing protocols and plans for more than 500 universities across America.
Would a phone app notify you if you were COVID-19 exposed?
This is the kind of thing that might not go over well with everybody, but you could imagine a university encouraging it.
A phone app called COVIDWise is being tested right now in Virginia that is both interesting and a tad creepy and invasive. You download the app and it keeps track of other people you come in contact with for a rolling 14 days. Everyone involved has to have the app loaded and on for this to work. Then, if you test positive, you tap the “alert” button and it notifies everybody who you came in contact with over the previous two weeks who also had the app that they may have been exposed. The app does not tell them who might have exposed them, where it happened or even when. It is just an alert to go get tested.
Washington Post staffers tried it out and could not prove it did or didn’t work. But they did discover that for an app like this to be of use, it would have to be used by about two-thirds of the population, which seems unlikely.
While this is only being tested in Virginia right now, the Association of Public Health Laboratories said it is working on a plan to expand the alert system.
One big downside is that all of the privacy protections built into the system also keep contact tracers from harvesting useful information.
The Harvard Business Review reminded us that some countries, including China, have required people to download contact tracing apps, which would not play well in the U.S. for sure. HBR said:
But in most countries where adoption is voluntary, the uptake has been low. For example, in Singapore, which guaranteed that adoption would be voluntary and that it would respect individuals’ privacy, only 35% of the population are using the app. In Iceland, the first country in Europe to launch its app (in early April), the adoption rate is still less than 40% as of July 8. And the adoption rates have been even lower in other European countries — despite the European Union issuing recommendations for a coordinated approach to design secure, protected, and interoperable contact-tracing apps in April.
Instead, HBR mentioned the notion of focusing requirements on high-risk communities. Imagine it would be a requirement to fly, attend school or enter a bar:
Instead of launching them broadly and indiscriminately, we should be deploying them in highly focused, contained, related communities, where they would be instantly useful: families, religious communities, workplaces, schools, bars and restaurants, beaches, hotels, trains, airplanes, and so on. In this way, the apps would have value immediately, and adoption within each small community might approach 100%. Once they gain critical mass in small communities, the apps can gradually be scaled and connected at the regional or national level.
I just keep thinking about conspiracy believers who would consider this one more way for somebody to track them. I can imagine a crime novel where a contract tracing app leads police to be able to prove the bad guys were near each other when the crime happened.
A possible game-changing cheap, noninvasive and fast COVID-19 test has been approved
The Food and Drug Administration has given emergency approval to a saliva-based COVID-19 test that is a lot less invasive than the swab test, costs about $10 and can be “turned around” in about 30 minutes, not days or hours.
The saliva test was developed at Yale University, which said production of the tests could be scaled up quickly. Yale announced:
This is a huge step forward to make testing more accessible,” said Chantal Vogels, a Yale postdoctoral fellow, who led the laboratory development and validation along with Doug Brackney, an adjunct assistant clinical professor. “This started off as an idea in our lab soon after we found saliva to be a promising sample type of the detection of SARS-CoV-2, and now it has the potential to be used on a large scale to help protect public health. We are delighted to make this contribution to the fight against coronavirus.” The preprint on the development and validation of SalivaDirect was recently posted on medRxiv.
The test, which also avoids a key step that has caused shortages of chemical reagents used in other tests, can run approximately 90 samples in fewer than three hours in a lab, although the number can be greater in big labs with automation.
“This could be one (of) the first major game changers in fighting the pandemic,” tweeted Andy Slavitt, a former acting administrator of the Centers for Medicare and Medicaid Services in the Obama administration, who expects testing capacity to be expanded significantly. “Rarely am I this enthusiastic … They are turning testing from a bespoke suit to a low-cost commodity.”
Yale’s saliva-based test also skirts a step that other COVID-19 tests require: extracting the virus’s genetic material. Extraction kits are one of many components of the existing diagnostic tests that have faced shortages. Supply issues have limited testing capacity overall, as well as slowed how quickly results can be returned.
The other advantage is that people can take their own samples by just spitting into a tube.
The test has an interesting beginning. The Verge explained that it started with NBA players:
The league is playing out the 2020 season inside a “bubble” at Disney World, and the NBA players there are tested for COVID-19 nearly every day. Players had the option of giving a saliva sample for SalivaDirect along with their swab test. The researchers then compared the two types of tests to make sure the saliva was just as accurate.
The NBA offered a ready-made group of people to study the method in. “What just made this really possible was that they already had staff out there collecting samples,” Anne Wyllie, the other project head, told The Verge in July.
Word of the week: “twindemic”
We cannot stop the pandemic without a vaccine, but we may be able to prevent a “twindemic,” which is a word I am seeing a lot this week. It refers to the one thing that worries health experts the most: a COVID-19 outbreak coupled with widespread seasonal flu.
Dr. Robert Redfield, director of the U.S. Centers for Disease Control and Prevention, is urging businesses to push employees to get flu vaccines as soon as they can. This year’s flu shots and nasal sprays started arriving at doctors’ offices and pharmacies last week.
“The private sector and CEOs can take a concrete step, play a big role in setting the example and have an enormous impact,” Redfield said. “The more we can prevent flu from causing hospitalizations, the more we can prevent people with flu from filling up our ICUs, the more probability that there is going to be a hospital bed for people with COVID.”
The New York Times reported that it may be more difficult for some people to avoid being vaccinated this year:
The flu vaccine is rarely mandated in the U.S. except by some health care facilities and nursery schools, but this month the statewide University of California system announced that because of the pandemic, it is requiring all 230,000 employees and 280,000 students to get the flu vaccine by November 1.
Dr. Anthony Fauci is imploring people to get the seasonal flu vaccine to keep hospitals from filling up with flu patients at the same time that there could be a new round of COVID-19 infections.
A physician friend of mine asked me to ask journalists not to say “flu shot,” but to instead call it a vaccine. “Shot” ignores the equally effective nasal spray that can be an appealing alternative for people who really hate shots. Though some people should not get the nasal spray influenza vaccine, including children younger than 2 years, adults 50 years and older and pregnant women.
15-cent movie tickets

An empty parking lot at the AMC Theatre in Clinton Township, Michigan. (AP Photo/Paul Sancya)
This Thursday, 100 AMC Theatres locations will reopen their movie screens by offering 15-cent movie tickets — the price of tickets when AMC opened its first theater in 1920.
The theatres have been closed because of the pandemic. The Hollywood Reporter said:
Around 300 additional AMC locations countrywide are expected to open over the following two weeks ahead of the theatrical release of Disney’s The New Mutants on Aug. 28 and Warner Bros.’ Tenet on Sept. 3. The AMC Theatres circuit, as it reopens in phases, will operate at reduced capacity to comply with local health restrictions amid the pandemic.
The remaining one-third of AMC’s U.S. theaters from early September are expected to open after being authorized to do so by state and local officials. After the relaunch on Aug. 20, AMC will screen throwback movie titles like Black Panther, Back to the Future, Ghostbusters and Star Wars: The Empire Strikes Back — with each movie priced at $5 per ticket, for screenings on dates other than Aug. 20.
And food and drinks at the concession stand will also be sold in part at reduced pricing through October.
A subdued COVID-19 Halloween
Halloween is big businesses for theme parks, haunted house venues and party/decoration stores. But 2020’s Halloween is likely to be way different. The National Retail Federation said, last year, the average shopper spent nearly $90 on Halloween stuff, which adds up to about $9 billion nationwide.
COVID will make costume parties less appealing, but then again maybe it is a way to get anti-maskers to try one on.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.
Al Tompkins is senior faculty at Poynter. He can be reached at atompkins@poynter.org or on Twitter, @atompkins.