Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
This is the question that worries everybody. What if you are vaccinated and then a new variant of the coronavirus shows up? Will you still be protected? The United Kingdom’s public health agency says it could be an issue.
The New York Times summarizes the situation:
The variant, known as B.1.1.7, first came to light in December. Researchers determined that it had rapidly become more common across Britain in just a couple of months.
Its spread appears to occur because of its improved ability to infect people. Experiments in test tubes suggest that some of its mutations allow the B.1.1.7 variant to hold on to cells more tightly than other coronaviruses.
Since B.1.1.7’s discovery in Britain, the variant has been reported in 72 other countries. The United States confirmed its first case of the B.1.1.7 variant on Dec. 29, but is conducting little of the genomic sequencing necessary to track the spread of new variants that have caused concern. Since then, the Centers for Disease Control and Prevention has recorded 467 samples of the variant in 32 states.
There is every reason to be concerned that these variants will directly confront our vaccination efforts.
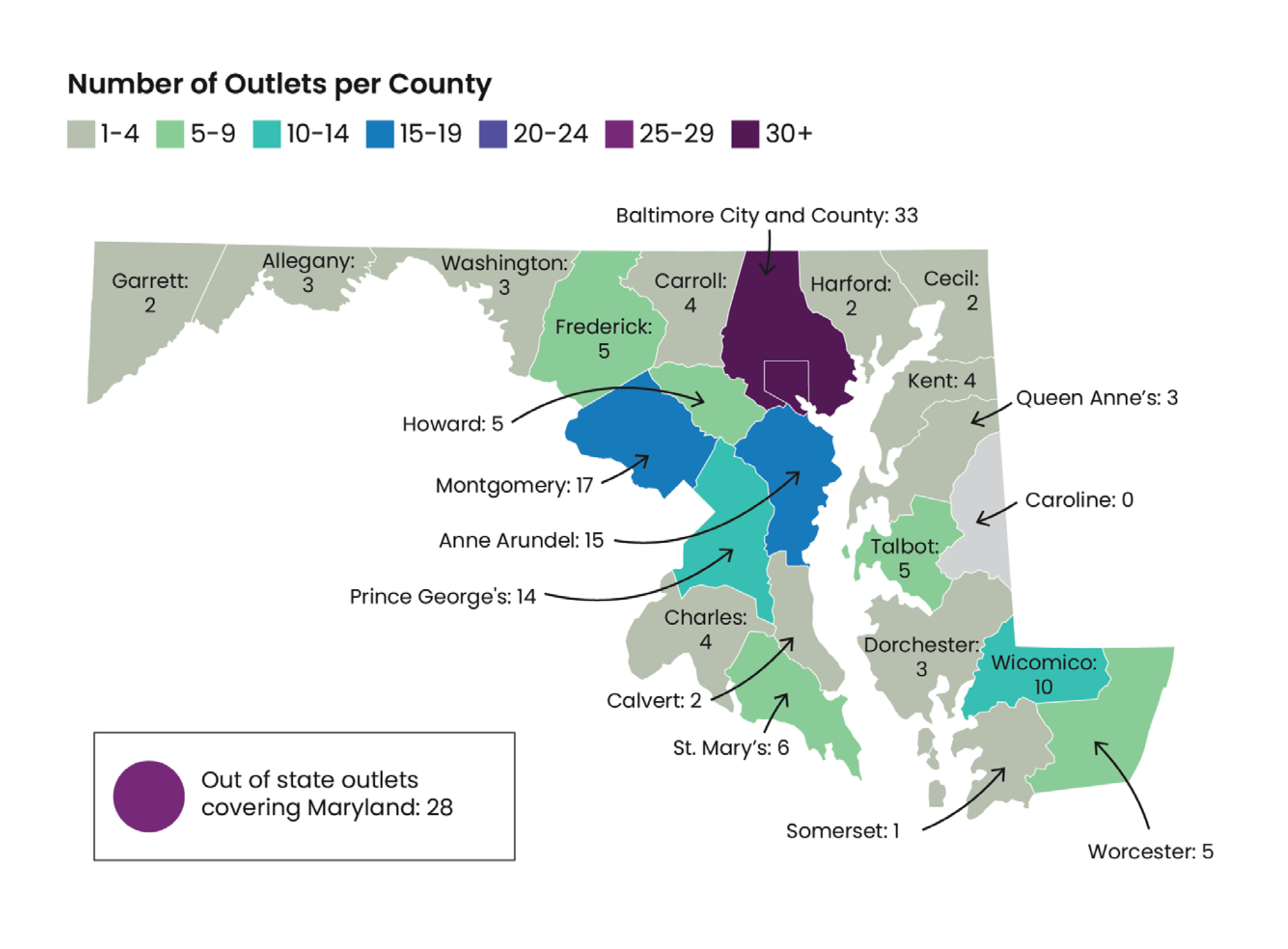
The Times points out that researchers in South Africa have found that two vaccines — one by Johnson & Johnson and the other by Novavax — are less effective against a variant called B.1.351, which has spread there. The South African variant is already in 31 countries including the United States, where it has been detected in Maryland and South Carolina.
If you have had COVID-19, do you need a second COVID-19 shot?
To quickly answer the question: Yes, even if you have had COVID-19, health experts still recommend you get both doses of the COVID-19 vaccine. But a new study says that if you have had the virus, you will likely have stronger reactions to the vaccine (including headaches, chills or muscle pain) because the vaccine is revving up your body’s existing immunity.
That study, by a virologist at the Icahn School of Medicine at Mount Sinai, also suggests that people who have had the virus may only need one dose of the vaccine. The Centers for Disease Control and Prevention and Food and Drug Administration have not weighed in on that yet.
The Icahn study tracks fairly closely to another from researchers at the University of Maryland. But again, that study only involved 59 health care workers, which is a long way from enough evidence to change national vaccine recommendations.
New data on the AstraZeneca vaccine suggests delaying the second shot longer

A health worker shows a vial of the Oxford-AstraZeneca vaccine for COVID-19 being used during a priority vaccination program for the elderly at a vaccination center in Rio de Janeiro, Brazil, Monday, Feb. 1, 2021. (AP Photo/Silvia Izquierdo)
The vaccine developed by AstraZeneca has not yet been approved for use in the U.S. But researchers say there is good reason to believe that there should be more time between the first and second shots of that drug.
The optimal time between shots may be three months, not one month as is currently believed. Researchers found that for drug trial participants who got two doses three months apart, the vaccine was 82% effective, compared to 55% when the doses were given less than six weeks apart. This is where I should tell you that that study has not been peer-reviewed so, again, the recommendation has a long way to go before it changes public policy.
If all goes as planned, the AstraZeneca vaccine could be available in the U.S. in a month or so.
Is there some connection between COVID-19 and diabetes?
There is not a ton of research yet, but it appears that COVID-19 might trigger Type 1 or Type 2 diabetes. Are the cases temporary or permanent? We do not know. One analyst says 14% of people who had severe cases of COVID-19 developed a form of diabetes. One hospital in Maryland is seeing twice as many diabetes cases compared to normal.
The Washington Post says one clue may be that so many severe COVID-19 cases also involve patients who have other chronic conditions, and that researchers have noticed this kind of thing before with SARS.
As early as January 2020, doctors in Wuhan, China, noticed elevated blood sugar in patients with covid-19. Physicians in Italy, another early hot spot, wondered whether diabetes diagnoses might follow, given the long-observed association between viral infections and the onset of diabetes. That association was seen in past outbreaks of other coronavirus illnesses such as SARS.
A year after the pandemic began, the precise nature and scope of the covid-diabetes link remain a mystery. Many of those who develop diabetes during or after covid-19 have risk factors, such as obesity or a family history of the disease. Elevated blood glucose levels also are common among those taking dexamethasone, a steroid that is a front-line treatment for covid-19. But cases also have occurred in patients with no known risk factors or prior health concerns. And some cases develop months after the body has cleared the virus.
Vaccines are heading to drugstores and grocery pharmacies in a new phase
You are already used to getting your flu shots at your local pharmacy so it won’t surprise you that the Biden administration says it will soon ship a million doses of the coronavirus vaccine to 6,500 pharmacies around the country. The one million doses will be in addition to the supplies that the drug companies send to states to be used at mass vaccination sites.
Some pharmacies are already administering vaccines, but those doses come out of the state’s supplies. CVS and Walgreens also have contracts to deliver shots at long-term care facilities. The vaccines should be delivered soon and shots will begin around Feb. 11. The pharmacies will follow state guidelines to determine who gets the vaccines.
The White House listed the retailers who will get vaccines. They include:
- Walgreens (including Duane Reade)
- CVS (including Long’s)
- Walmart (including Sam’s Club)
- Rite Aid
- Kroger (including Harris Teeter, Fred Meyer, Fry’s, Ralphs, King Soopers, Smiths, City Market, Dillons, Mariano’s, Pick-n-Save, Copps and Metro Market)
- Publix
- Costco
- Albertsons (including Osco, Jewel-Osco, Albertsons Market, Safeway, Tom Thumb, Star Market, Shaw’s, Haggen, Acme, Randalls, Carrs, Market Street, United, Vons, Pavilions, Amigos, Lucky’s, Pak n Save and Sav-On)
- Hy-Vee
- Meijer
- H-E-B
- Retail Business Services, LLC (including Food Lion, Giant Food, The Giant Company, Hannaford Bros Co and Stop & Shop)
- Winn-Dixie (including Harveys and Fresco Y Mas)
A free, open-source database on deaths at 523 jails
Pete Eisler at Reuters is giving journalists a great gift that I suspect will produce a ton of stories. Eisler and his colleagues produced a huge investigation called “Dying Inside” which, for the first time, examined who is dying in America’s jails and why.
The team filed 1,500 public records requests for data from 523 jails around America. They looked at the 10 largest jails in each state plus all jails with more than 750 people locked up. They pulled the records for every death that occurred from 2008 through 2019. Keep in mind this does not include COVID-19 deaths.
Eisler has now released the data for you to explore.
Here is what you will find in the data:
The surge in deaths comes as jails grapple with inmate populations racked by sickness, mental illness and addictions that often go unaddressed behind bars. More than a quarter of the deaths documented by Reuters were suicides. More than 1 in 10 last year were tied to the acute effects of drugs and alcohol.
Reuters documented 7,571 inmate deaths at 523 American jails from 2008 to 2019. The mortality rate in those local lockups climbed 8% over the last three years and 35% over the decade ending in 2019. Problem jails are masked by a secretive federal reporting system and scant oversight by local, state or federal agencies.
At least two-thirds of the dead, 4,998 people, died awaiting trial, never getting their day in court for the charges they faced. Nearly 300 inmates spent a year or more jailed, never convicted of the pending charges, before their deaths.
Sixty-two percent of top U.S. jails have privatized their healthcare services. It has been a deadly shift. From 2016-18, jails in the Reuters survey that hired one of the five dominant jail healthcare companies had average death rates from illness, suicide or drug- and alcohol-related problems 18%-58% higher than jails with inmate healthcare managed by public agencies.
Undocumented women are among the most vulnerable to COVID-19. How do we reach them?
The 19th’s Shefali Luthra and Chabeli Carrazana bring us the story of undocumented workers who have no insurance coverage and work on the front line of COVID-19 health care: home health.
Their reporting includes this insight:
Though coronavirus testing, treatment or vaccination don’t count against permanent residency, the distinctions of what programs do count and which don’t are difficult to communicate. The Trump administration, experts note, never worked to clarify that immigrants would not be penalized for seeking coronavirus care. Now, many worry that message could carry over to immigrants weighing a coronavirus vaccine, regardless of their legal status.
“They might be fearful that by somehow putting their name on a list of people getting a vaccine, that might trigger some exposure that would compromise their ability to stay in the U.S.,” said Shelby Gonzales, director of immigration policy at the Center for Budget Policy and Priorities, a liberal think tank in D.C. “They may fear accessing a vaccine that is free … is getting a public benefit that later on will put them in harm’s way when they seek to adjust their status, or seek to bring somebody to the U.S. from outside of the country.”
Undoing the climate of fear will take deliberate outreach from the Biden administration, but there is also a need for concerted on-the-ground organizing and communication, experts said.
Pay close attention to this next passage from their reporting. It is something all journalists should explore:
There are also language barriers that can make it harder for people to book a vaccine appointment, said Haeyoung Yoon, senior policy director for the National Domestic Workers Alliance. Many of the systems states use to sign people up for vaccination appointments are primarily in English, or connect users to vaccine coordinators who don’t speak their native language, she said.
Because of this, advocates and health disparities researchers worry many women will end up at the back of the line, even while they are working in jobs with higher risk of coronavirus exposure.
A pandemic snowmobile shortage?

A person on a snowmobile rides on a trail, Saturday, Jan. 23, 2021, in Rangeley, Maine. (AP Photo/Robert F. Bukaty)
We had a shortage of bicycles for sale last spring and summer. Now there is a run on snowmobiles. The cause is the same — people are stir-crazy from the pandemic.
The Associated Press has this quote, which seems to say it all:
“We’ve had some good years and some bad years, but we’ve never had anything quite like this one,” said Dave Jones at Jackman Powersports, who expects to sell about 450 snowmobiles this year.
Nearly a third of sales were to new riders, Jones said, and he would sell more snowmobiles if he could get more from manufacturers.
The Michigan-based International Snowmobile Manufacturers Association says snowmobile sales are expected to increase 15 to 20% this winter, the most since the winter of 1995-96.

(ISMA)
Here is way more data than you could reasonably want on snowmobiles in the U.S. and Canada.
Snowmobile sales in Florida are apparently flat year to year.
Travel trailers with built-in offices
If my wife asks you, yes, I would like to have one of these. But they cost more than $100,000, so there is that. RVs are selling fast right now.
The pandemic boosts ‘payment wearables’

This Oct. 8, 2019 file photo shows the Apple Pay app on an iPhone in New York. (AP Photo/Jenny Kane, File)
Jennifer A. Kingson at Axios explores the rise of things you wear on your wrist that act as credit or debit cards. The pandemic has encouraged people to use these devices rather than touch keypads or hand over cards.
The day is coming that you won’t have to wear your payment method, but instead will be able to wave your hand under a reader:
Amazon is expanding use of its “Amazon One” payment terminals — which read your palm to authenticate a transaction. Under Amazon’s vision, a biometric identifier — the palm image — would become a ubiquitous payment vehicle.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.