Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
We will know soon whether Johnson & Johnson’s version of a coronavirus vaccine works as well as the two vaccines already in use. But this is not just another vaccine. It is way different.
First, Johnson & Johnson, by its sheer size, would be able to produce, it says, maybe a billion doses by the end of 2021.
And, unlike the already approved drugs, the Johnson & Johnson vaccine is a single dose. Think of it this way: It would take 2 billion doses of the Moderna and Pfizer two-dose shots to vaccinate the same number of people.
The company says it is in the “final stages” of analyzing the phase 3 trial involving 45,000 patients. If all goes well, Johnson & Johnson may go before the U.S. Food and Drug Administration on Jan. 21 for emergency authorization.
Barrons frames the anticipation for these results this way:
Unlike the vaccines from Pfizer (PFE) and Moderna (MRNA), which require a two-dose regimen, the Johnson & Johnson vaccine is being tested in a single-dose formulation. The vaccine also is not subject to the same cumbersome storage requirements as the two authorized vaccines.
“The JNJ data could be the most influential event of the month given its potential impact on the market and on (Moderna) and (Pfizer) as first-to-market players,” wrote Jefferies health-care trading-desk analyst Jared Holz in an email to investors on Monday. “JNJ, as a single injection that has a less cumbersome supply chain around it, could be very important.”
HHS says give vaccines to persons over age 65
The Department of Health and Human Services says vaccines should go to people over age 65 and to all adults who have preexisting conditions that put them at a greater COVID-19 risk. It may not sound like much news to those of you whose states have already made such a move, but that’s sort of the point. We have, essentially, 50 different messages coming from states and territories because the rollout is all state-controlled.
The bigger issue is how to make the process of administering the shots more efficient and orderly.
Axios collected a list of mega-sites like stadium and fairground parking lots that some states will be using. In Arizona, the site is slated to be open 24/7.
In New York, seniors face a 51-step COVID-19 vaccine registration process
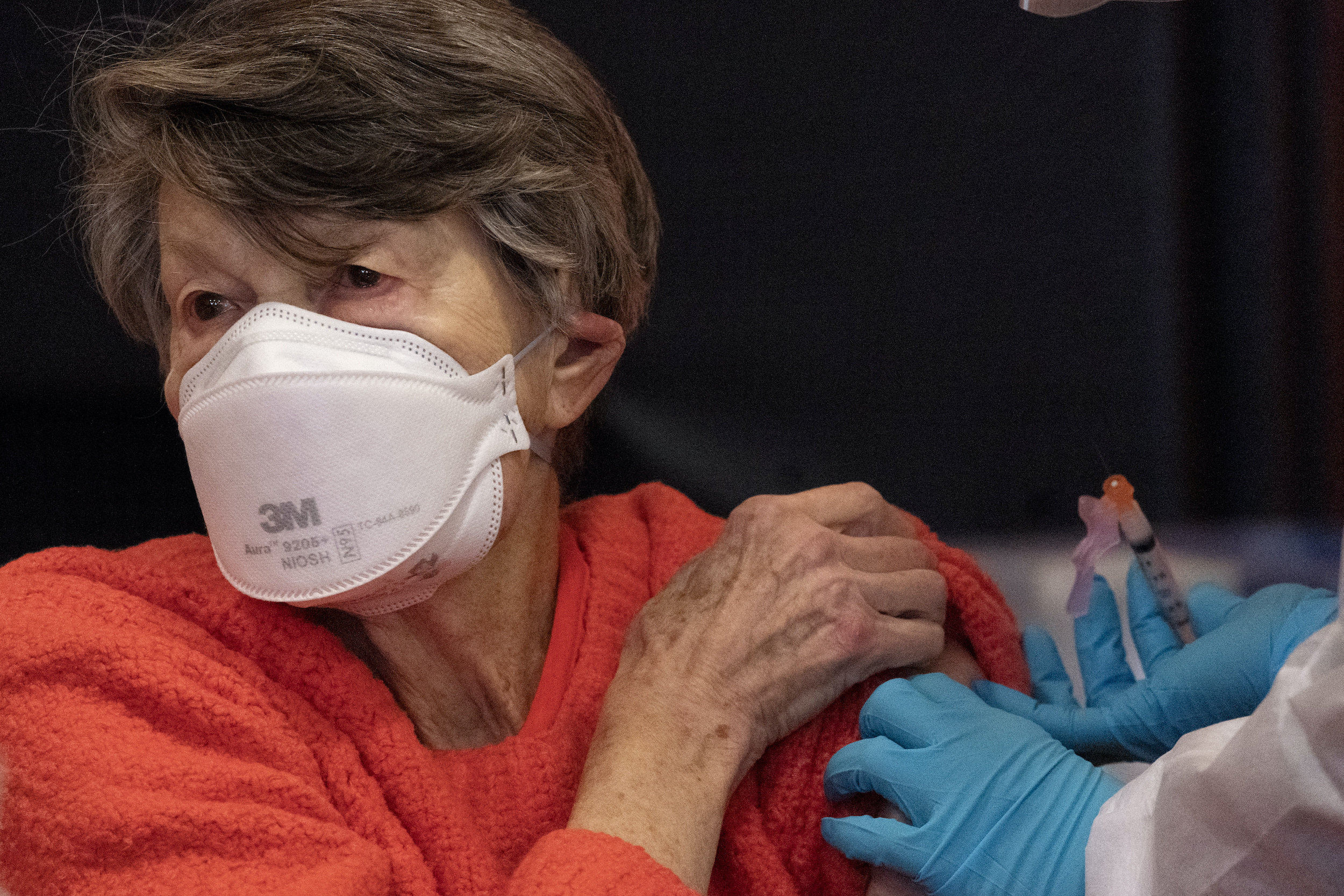
Renee Dunn, 84, gets the coronavirus vaccine at a clinic organized by New York City’s Department of Health, Monday, Jan. 11, 2021. (AP Photo/Mark Lennihan)
I thought the Florida Department of Health’s registration process to get COVID-19 shots was the ultimate disaster but, compared to the 51-step registration in New York, we have it easy.
“The @nychealthy site has a multi-step verification process just to set up an account, and then a six-step process to set up an appointment,” (New York City Comptroller Scott) Stringer wrote, after having attempted to navigate the digital portal himself. “Along the way, there as many as 51 questions or fields, in addition to uploading images of your insurance card.”
“All of this will be particularly challenging for populations that struggle with digital literacy and digital access — who have been hit hardest by this pandemic and who need the vaccine most,” the comptroller continued. “We can’t force frontline workers and those over 75 to confront a bewildering signup process. Any barrier to getting shots in arms is only going to prolong the agony of this crisis.”
Take a few minutes and watch this piece from CBS “Sunday Morning” in which contributor Josh Seftel tries to talk his mother through registering for the vaccine in Florida.
An Associated Press story reports:
Detroit’s call center was jammed with more than 100,000 calls Monday as the city took appointments for vaccinations at the city’s TCF convention center, starting Wednesday. Officials plan to schedule 20,000 appointments over the next month for elderly people. Police officers and bus drivers can start getting shots there at the end of the week.
“We do not have the capacity to answer questions from people under 75 or non-Detroiters about vaccinations in general,” said Detroit’s chief operating officer, Hakim Berry. “If you are not eligible, please do not tie up the call lines.”
In New York City, two round-the-clock sites opened and several more are expected to be up and running over the next two weeks. Appointments for the midnight-to-4-a.m. shift on Tuesday were snapped up quickly in what Mayor Bill de Blasio pointed out is, after all, “the city that never sleeps.”
Moderna vaccine may last ‘at least a year’
Moderna says now that its vaccine may protect you for a year. This story is an incremental step in understanding how long the COVID-19 vaccines might protect you.
If you think about the implications, they are profound. If the virus keeps morphing, and it will, will we need to get annual booster shots for this virus in addition to our flu vaccines? If we fail, how quickly might this virus reestablish itself? The answers will reveal themselves over time as the first drug trial participants give us data well ahead of the rest of the population. But if we learn, for example, that we need annual (or thereabouts) boosters, the response will need to be nimble and global.
When is eating ‘outside’ really no safer than eating ‘inside?’

A restaurant with an “outdoor” dining area in New York City. (Photo: STRF/STAR MAX/IPx)
The winter of 2020-21 is a season of outdoor eating, under the premise that eating outdoors is safer than everyone being in the same dining room. But experts say we may be kidding ourselves. We are really just building rooms outdoors that act just like dining rooms. Let’s turn to Popular Science for this one:
But when it comes to COVID transmission, does eating in your own personal hamster ball, igloo, or dog house count as eating outside? According to Marissa Baker, an assistant professor at the University of Washington’s public health school who specializes in industrial hygiene, it really depends.
Popping outdoor diners under tarps to keep out the sun and rain during warm weather is one thing—if air is still freely flowing, you get most of the benefits of being outside. But as temperature control becomes more of a concern, those “outdoor” structures can quickly turn into “indoor” environments.
“It seems like as it’s gotten colder and wetter, you’re seeing structures getting more elaborate,” Baker says. And once you’ve put up four walls and a roof, you might as well just seat people inside. Even if those walls are made of vinyl instead of drywall, you’re still not getting the airflow you need to reduce the risk of viral transmission.
Popular Science goes over the main outdoor dining structures and rates them worst to best in terms of COVID-19 safety. Suffice it to say, the more open, the better. And then there is always takeout.
Do-it-yourself contact-tracing
Kaiser Health News ran an interesting piece about how health departments that are short on staff are urging people who test positive for COVID-19 to do their own contact-tracing.
Asking infected people, some of whom might be sick, to call their own friends and families — in effect, conduct their own contact-tracing operation — is far from ideal, public health experts said.
“It is a last-resort tool,” said University of Michigan public health professor Angela Beck. “It is the best that we can do in the situation that we’re in, but it’s a compromised strategy.”
Contact tracing is more than just alerting people to a potential exposure so they can quarantine. Part of the process is to conduct carefully structured interviews with those exposed, to determine if they’ve developed symptoms of covid-19. If so, contacts of those people also need to be traced and told to quarantine, to prevent the virus from proliferating through successive chains of people in the community.
The community fridge movement
In some communities, brightly colored refrigerators called community fridges are showing up on sidewalks. They almost always are run by volunteers and are stocked with food and other supplies. This one is new to me but, for some of you, it has been around a while, especially during the pandemic. Mashable reports:
Community fridges are much more than charity or interesting sidewalk art. They’re a prime example of bottom-up, mutual aid initiatives that put resources directly into the hands of communities that need them the most, veering from the model of charity-based food programs, which put the “power” of resource allocation into the hands of the few and often have criteria for who receives aid. As Free99Fridge, a network of “solidarity” fridges in Atlanta, explains on their site, “This differs from a traditional charity, with the goal of empowerment.”
The beginnings of the community fridge movement are often credited to European food-sharing initiatives, like the Foodshare program started in 2014 in Berlin, Germany. What began as an anti-food waste movement quickly expanded. Freedge, an international network established in 2014 to promote and support community fridges, documents their use on every continent except Antarctica, and at least 200 registered fridges across the United States.
The current food sharing movement in America is a response to growing food insecurity, made worse this year by financial insecurity caused by COVID-19. According to research by Feeding America, the nation’s largest nonprofit hunger relief organization, more than 50 million Americans were estimated to face food insecurity during 2020. With COVID-19 cases continuing to climb, community fridges can provide another safe way to volunteer while staying close to home.
There are a variety of models — ones that operate within larger city-wide networks, like those within Los Angeles Community Fridges, a decentralized network of community fridges run by volunteers, and A New World In Our Hearts NYC, as well as those stocked, cleaned, and managed by individuals.
Mashable provides a step-by-step guide on how to get these started. Some of them are incredibly thoughtfully run and include an online monitoring system that is, by the way, bilingual.
They are not everywhere but you can find them in Davis, California; Minneapolis; Washington, D.C.; New York; Los Angeles; Ft. Collins, Colorado; and Saskatoon, Canada. I have even seen mention of one here in little old St. Pete. Here is a map.
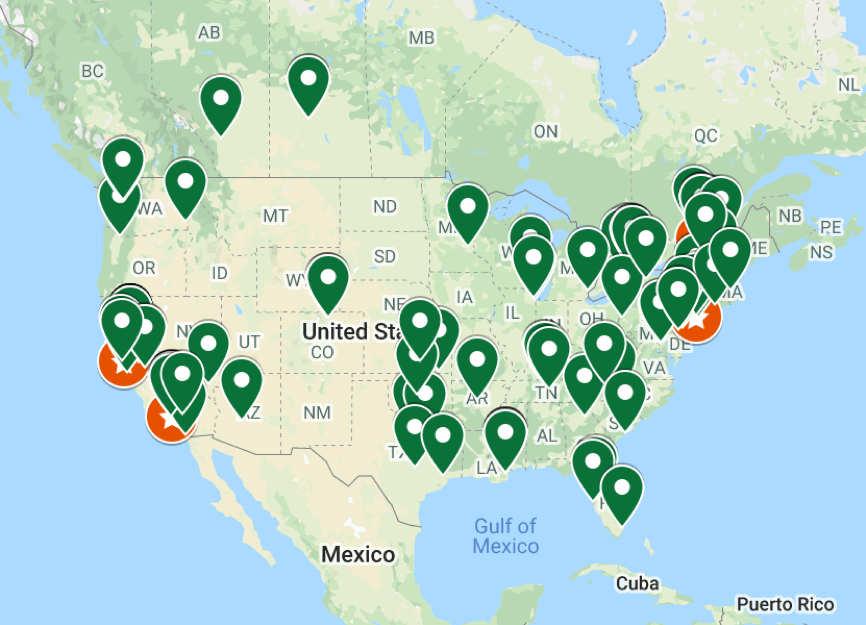
(Freedge)
Dentists giving COVID-19 vaccines
This makes sense to me. In California and Oregon, dentists are now giving COVID-19 vaccine shots. At least 20 states are considering recruiting nontraditional providers, including students, dentists, veterinarians and paramedics.
NCAA delays vote on compensating college athletes
How about a non-virus story that touches virtually every media market in some way?
The NCAA Division I Council was supposed to vote this week on allowing college athletes to be paid. But there was no vote Monday, when everyone thought it would happen, and we have not heard when it will come back up. The delay puts any hope of getting compensation in place by this fall in jeopardy.
NCAA President Mark Emmert told The Associated Press on Saturday that he recommended to the association’s two top governing bodies to put off votes on name, image and likeness and the transfer proposals because of a letter he received from the Department of Justice about potential antitrust violations.
Under the NCAA’s current proposal, schools could block athletes from entering sponsorship agreements that conflict with their schools’ deals. For example, an athlete at a school associated with Nike could be prevented from entering an agreement with another shoe or apparel company. Also, athletes would not be permitted to endorse products or companies such as alcohol or gambling that conflict with NCAA values.
The NCAA’s proposed NIL legislation would allow athletes to strike financial deals with third parties to do things like endorse or sponsor products, make personal appearances or be an online influencer. Schools would not be involved in the compensation.
Six states have passed bills allowing college athletes to cash in on their names, images and likenesses. Florida’s law is scheduled to go into effect in July. The hope has been for athletes to begin participating in NIL compensation in August.
How much money are we talking about here? CNBC reports some fairly stunning estimates:
A new study from the National Bureau of Economic Research looks to get to the bottom of just how much money the top college football and basketball stars would be making per season if they were compensated similarly to professional players, whose collective bargaining agreements with professional leagues assure them a roughly 50% share of league revenue.
According to the study, paying college stars similarly to professional players (by sharing half the revenue from their games, and paying high-profile players a higher percentage) would mean that top quarterbacks, like Clemson’s preseason All-American signal caller Trevor Lawrence, would earn up to $2.4 million per season, on average. A star wide receiver would earn up to $1.3 million per year, according to NBER.
The study also found that every starting player on a basketball team for schools in the five biggest collegiate athletic conferences (the ACC, the Big 10, the Big 12, the PAC-12 and the SEC) would earn between $800,000 and $1.2 million per season, depending on their school and the percentage of revenue that was shared with each player.
We’ll be back tomorrow with a new edition of Covering COVID-19. Sign up here to get it delivered right to your inbox.