Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
In theory, over the weekend, your health insurance was to have begun covering the cost of instant COVID-19 tests. President Joe Biden announced the plan last week that would allow Americans to get tests without spending money, since at-home tests typically cost $15 — or sometimes a lot more, if you can find one.
But insurance companies say they are not ready and that they won’t be, maybe for weeks. The problem is that it takes time to write the billing codes that insurers use to process payments. Rather than picking up test kits and walking out of the store without paying anything out of pocket, lots of people will likely pay out of pocket, save up their receipts and send them to the insurance company for payment. It might take a while, at least until the system gets ironed out. The New York Times reports:
“This is taking things back to the olden days, where you’ll have a person throwing all these paper slips in a shoe box, and eventually stuffing it into an envelope and sending it off to a health insurer to decipher,” said Ceci Connolly, president and C.E.O. of the Alliance of Community Health Plans, which represents smaller, nonprofit insurers.
“There will be some people who buy them, and then have a six-month nightmare trying to get reimbursed,” said Jenny Chumbley Hogue, a Texas-based insurance broker. She has not yet seen a plan she works with that has sent out member guidance on how coverage will be handled.
Uncertain of what the rules will be, Ms. Hogue is advising her clients to save not just receipts but also the boxes that the tests come in, because some plans may require the boxes as proof of purchase.
Even the White House issued a statement that says, yes, you may have to send paperwork to your employer to get your payment. “If Americans are charged upfront, it is important that they keep their receipts and be prepared to submit them for reimbursement. The most important thing is that starting Saturday those tests are covered free of charge.”
The Biden order says insurance will reimburse up to eight over-the-counter at-home tests per month with no deductibles or cost-sharing. The kits I bought have two tests in them — the government will include multiple test boxes as a single test for reimbursement purposes. If a doctor tells you to take a test, that does not count as one of the eight. Make sure whatever test you use is one of these Food and Drug Administration-approved tests. The reimbursement will not apply to a test that is not FDA-approved.
Sometime in the next couple of weeks, Biden says, the government will be ready to send a half-billion home tests to people who ask for them.
By the way, any tests that you bought before Saturday are on your own dime.
You probably need at least two negative test results to feel confident
There is a good reason why rapid tests come in packs of two. If you test one day and and get a negative result, test again in a day or two. Rapid tests may not pick up an infection that you caught only a day or two before. Then tests are also more accurate in picking up positive results in people who have COVID-19 symptoms. In summary, if you think you were exposed or you feel symptomatic, take a test. If you get a negative result, good for you. Wear a mask outside your home and test again tomorrow.
Jails and prisons are again swamped with COVID

The Palm Beach County Main Detention Center is shown, Friday, June 4, 2021, in West Palm Beach, Fla. (AP Photo/Wilfredo Lee)
I am again seeing local stories nationwide about COVID-19 outbreaks in county jails and prisons. From rural Texas to Connecticut, outbreaks are infecting staff at the same time that the facilities struggle to hire people to fill big staff vacancies.
In Coconino County, Arizona, the local detention facility is not accepting people charged with nonviolent misdemeanor arrests to try to create more distance between people in lockup and slow the spread of the coronavirus.
In King County, Washington, KIRO radio reports:
The president of the King County Corrections Guild is calling for a two-week shutdown of all jail operations.
There are just over 1,300 inmates in custody in King County. KCCG President Dennis Folk says nearly 34% totaling 460 inmates are either COVID positive or in COVID protocols. There are also 40 staff members in the same situation. That’s led to tense situations among prison populations in the county.
WISC-TV in Madison, Wisconsin reports:
About 6% of the state’s 20,000 prisoners have an active COVID-19 infection as of January 12, according to data from the DOC. That’s a sharp increase since vaccinations started; active cases largely remained in the single or low-double digits throughout the summer and fall of 2021 before beginning to creep upwards in December.
The largest outbreak is at New Lisbon, where nearly 500 inmates have an active infection.
33 prisoners in Wisconsin have died from COVID-19 since the pandemic began. Prisons and jails are once again limiting visitations. Wisconsin just announced such a plan. WISC explains:
The restriction applies to attorneys and other types of professional visits, as well as outside contractors, volunteers, maintenance, and any other types of non-DOC staff. Religious and emergency personnel are an exception but will need to take a rapid test before entry starting January 18.
Two people being held in Connecticut prisons died from COVID-19 last week. Out of concern about spreading infections, the Illinois prison system stopped accepting newly convicted inmates from county jails.
In Sacramento, the sheriff is releasing 200 prisoners to try to slow the spread of the virus through the county’s lockups. One facility counted 76 infections and another tallied 48 cases. The Guardian reported on the situation in California that is being repeated nationwide:
Staff infections increased 212% in January with more than 3,800 active cases in dozens of state facilities. The surge comes amid debate over a federal judge’s order that all prison staff must be vaccinated, a mandate facing legal challenges from the governor and the corrections officer union.
Currently, 69% of prison workers are fully vaccinated, according to the California department of corrections and rehabilitation, although the percentage varies drastically from prison to prison. At three facilities, fewer than 50% of staff are fully vaccinated, according to the department.
The Federal Bureau of Prisons says:
There are 3,761 federal inmates and 922 BOP staff who have confirmed positive test results for COVID-19 nationwide. Currently, 42,275 inmates and 8,902 staff have recovered. There have been 275 federal inmate deaths and 7 BOP staff member deaths attributed to COVID-19 disease. Of the inmate deaths, 11 occurred while on home confinement.
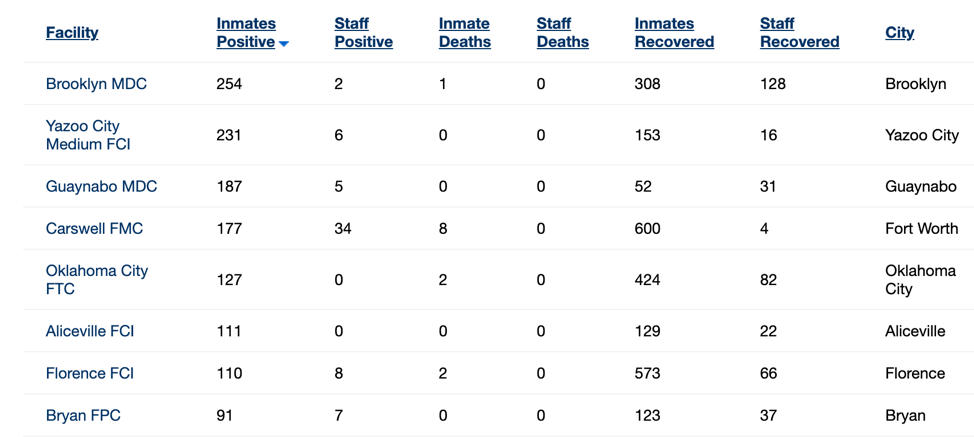
This is the BOP’s dashboard. It gives you an idea of how federal prisons are tightening operations in the face of the newest outbreak:
You can use the dashboard to get a facility-by-facility breakdown of COVID-19 cases.
This BOP map provides an idea of the size of the problem. The number on the map represents the facilities in each state that have active COVID-19 cases. Just click on the number and drill down on the facilities.
Here are some of the federal facilities that have the most infected prisoners and staff. Notice, for example, at one prison in Ft. Worth, Texas, there are 177 infected prisoners and 34 infected staff workers.
When the pandemic began, jails and prisons were so overwhelmed by COVID-19 that some states and counties sent incarcerated people home to serve their sentences. But when the pandemic retreated in 2021, states started locking people up again.
County jails, like the one in Minnehaha County, South Dakota (Sioux Falls), conduct multi-level screenings for every person who comes in. That jail is one example of a facility that cut its population but now has more prisoners than before the pandemic. The Argus Leader reports:
According to an analysis of COVID-19 data from the South Dakota Department of Corrections, the total active cases among inmates across state prisons reported as of Jan. 4 stood at 73 – more than five times the total number of active cases reported from the month prior.
Some of the initiatives that tracked prisoner and staff infections stopped tracking new outbreaks, so it is difficult, right now, to get reliable data, which makes your local reporting all the more important.
The head of the Federal Bureau of Prisons, Michael Carvajal, is resigning just as cases are rising.
The Prison Policy Initiative put it this way:
From the beginning of the pandemic, it was clear that densely packed prisons and jails — the result of decades of mass incarceration in the U.S. — presented dangerous conditions for the transmission of COVID-19. More than a year later, the virus has claimed more than 2,700 lives behind bars and infected 1 out of every 3 people in prison.
Millions of families just stopped getting monthly tax credit checks
It is not a surprise that the monthly tax credit payments to millions of Americans stopped last week. The American Rescue Plan hatched last March was not intended to go on forever, although some Democrats pushed and are still pushing for a version of it to continue. If they had been able to pass President Biden’s Build Back Better Plan, payments would have hit bank accounts over the weekend. But families are starting the first week of 2022 without the financial boost they have relied on for six months.
The tax credit provided up to $1,800 in monthly payments per child aged 5 and younger, and up to $1,500 for kids between ages 6 to 17. The Congressional Budget Office estimates it would cost $185 billion for one year, as Build Back Better proposes, or $1.6 trillion over the next decade if it continued beyond the first year.
Various polls find that while the majority of people who identify as Democrats support the tax credits, Independents and Republicans do not.
Parents interviewed by CBS MoneyWatch said they are planning to cut back on essentials like food as well as expenses such as cable TV to try to cope with the double-whammy of inflation on top of the expired benefit. Many worried about the impact on their children.
Anti-poverty experts say the impact on children could be extreme. Without the continuation of the monthly payments, about 10 million children are at risk of slipping into poverty, according to a recent estimate from the Center on Budget and Policy Priorities (CBPP).
By the way, people who got the Advance Child Tax Credit payments will soon get something called a Letter 6475. They will need that document when they file their 2021 tax return. Some will discover that they got more advance payments than they were due, and the IRS will demand they repay the overpayment.
Puerto Rico to require booster shots for public school students over age 12
Puerto Rico’s positivity rate was running below 5% just a few weeks ago. Now it is 36%, and Gov. Pedro Pierluisi says it is time to mandate booster shots for his highly vaccinated island population.
Pierluisi tweeted that people who work in hotels, cinemas, and convention centers, among other sectors, will have to get boosters as well as college and technical degree students.
The governor said people who seek a medical or religious exemption will have to take regular COVID-19 tests.
Doctors and nurses forced to work even if they test positive
The practice is happening across the country.
- In New Jersey, a nurse was recently instructed to come to work despite concerns that she had contracted Covid-19, according to a union representative.
- In Rhode Island, a nursing home and state-run hospital system recently used workers who tested positive after the state updated its guidelines in accordance with the CDC.
- In Missouri, a hospital is bringing back nurses after five days as long as they are asymptomatic. Health care workers around the country have reported that they are being called in to work even if they suspect they are infectious.
In interviews with several hospital executives, health care workers and health officials, nearly all said they are following the CDC’s new advice.
Let’s drill in on the CDC guidance. The guidance, released last month, allows facilities to bring back workers after five days of isolation, instead of 10, without a negative COVID-19 test. In cases where workforce shortages become extreme, hospitals can bring back staff without any isolation period.
California health authorities announced (a week ago) that hospital staff members who test positive but are symptom-free can continue working. Some hospitals in Rhode Island and Arizona have likewise told employees they can stay on the job if they have no symptoms or just mild ones.
Here is the decision grid that the CDC issued. It offers a sort of sliding scale of when to bring infected workers back according to how dire the need is. (HCP is short for health care professionals.)
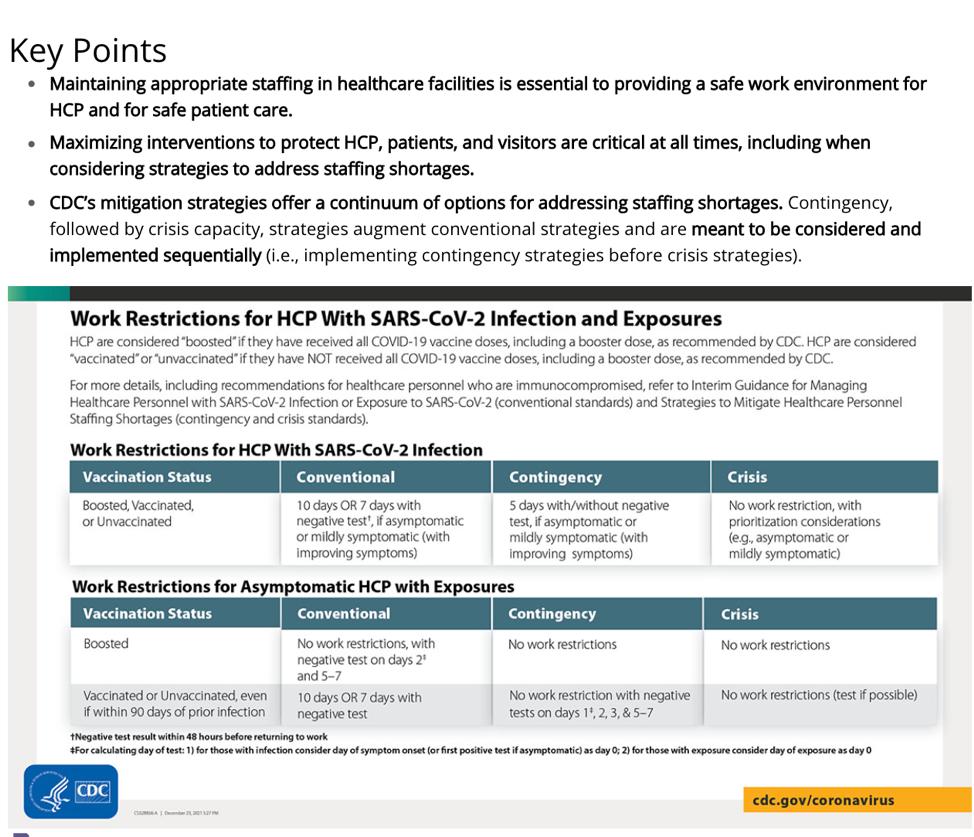
(CDC)
Spain compensates health care workers for not having enough protective gear during pandemic
Health care workers in the United States may be interested to know that one region in Spain is going to give doctors $56,000 each for having to work without protective gear during the early part of the pandemic. Of course, we had many instances in the U.S. in which doctors and nurses reused personal protective equipment, supplied their own or made do with whatever they could find.
Hiring the homeless to take a COVID-19 shot
Canada’s Globe and Mail reports:
Homeless and vulnerable people in British Columbia and Alberta have been approached with offers of payment to be vaccinated against COVID-19 by those attempting to fraudulently get a vaccine card.
Vancouver Coastal Health said Thursday those who have been approached have been asked to get vaccinated while falsely using that person’s name and information.
We’ll be back tomorrow with a new edition of Covering COVID-19. Are you subscribed? Sign up here to get it delivered right to your inbox.