Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Covering COVID-19 is a daily Poynter briefing of story ideas about the coronavirus and other timely topics for journalists, written by senior faculty Al Tompkins. Sign up here to have it delivered to your inbox every weekday morning.
Starting Saturday, your private health insurance plan will have to pay for eight at-home COVID-19 tests per month.
The Biden administration released the new rule late Monday and said it will provide incentives for insurers to cover these costs upfront. They will not require a referral from a physician, as you would a prescription.
The announcement, from the Department of Health and Human Services, said, “The new coverage requirement means that most consumers with private health coverage can go online or to a pharmacy or store, buy a test, and either get it paid for up front by their health plan, or get reimbursed for the cost by submitting a claim to their plan.”
About 45% of the U.S. population is covered by private health insurance, so the order affects about 150 million Americans.
The Center for Medicare and Medicaid Services said:
Beginning January 15, 2022, individuals with private health insurance coverage or covered by a group health plan who purchase an over-the-counter COVID-19 diagnostic test authorized, cleared, or approved by the U.S. Food and Drug Administration (FDA) will be able to have those test costs covered by their plan or insurance. Insurance companies and health plans are required to cover 8 free over-the-counter at-home tests per covered individual per month.
That means a family of four, all on the same plan, would be able to get up to 32 of these tests covered by their health plan per month. There is no limit on the number of tests, including at-home tests, that are covered if ordered or administered by a health care provider following an individualized clinical assessment, including for those who may need them due to underlying medical conditions.
Over-the-counter test purchases will be covered in the commercial market without the need for a health care provider’s order or individualized clinical assessment, and without any cost-sharing requirements such as deductibles, co-payments or coinsurance, prior authorization, or other medical management requirements.
Of course, all of this doesn’t help much if you can’t find tests to buy. Some retailers are limiting how many you can buy at a time, and CBS News says others are hiking prices:
Tanga, an online retailer that sells an array of products, usually at a discount, is now offering BinaxNow home COVID-19 test kits for $59.99 (one box containing two tests) and $349 for 10 boxes. Walmart sells the two-test BinaxNow kit for $19.88, but it’s out of stock. At Walgreens, the kit sells for $23.99.
The new order will not retroactively cover at-home tests you have already purchased.
This announcement is in addition to President Joe Biden’s plan to deliver 500 million free at-home tests later this month, although those plans are still pending.
Why are there no Braille COVID-19 rapid tests?
Bravo to The New York Times for its piece on how people who are blind have no Braille version of rapid COVID-19 at-home tests. The story said:
Some blind people manage to take at-home tests with the help of video call apps, like Be My Eyes and Aira. These services pair blind individuals with a sighted person who can describe their surroundings and guide them through a test, step by step.
But these interactions are difficult, and not everyone who is blind owns a smartphone or is able to use a smartphone. What’s more, relying on others can erode a blind person’s privacy and independence.
“It’s your personal health information,” said Martin Wingfield, the head of brand at the Royal National Institute of Blind People in Britain. “You should be the first to know.”
There are home-pregnancy tests that deliver results through Braille-like bumps, so the technology does exist, but they cost more than $20. There are some services that come to a patient’s home and administer COVID-19 tests, but you generally have to live in a big city to have access.
The Centers for Disease Control and Prevention says a million Americans are blind, 3 million have a severe visual impairment, vision loss is among the top 10 disabilities in the U.S., and the number of people with vision loss is growing. Get state-level data here.
The new best-case and worst-case COVID scenarios
Researchers at the University of Texas estimated that the United States might see 230,700 COVID-19 cases per day in January as a best-case scenario and 552,400 cases per day as a worst-case scenario. We have blown past those estimates.
Now, the researchers have updated the forecast. Keeping in mind that the current seven-day average of new cases is 656,000, the UT COVID Modeling Consortium says even the best-case scenario is still worse than what we have today:
Best case scenario: By January 13, an average of 766,800 people catch the virus every day—about 20% higher case rate than yesterday. In this scenario, Omicron would lead to a peak of 17,700 daily hospital admissions and 1,700 deaths per day.
Worst case scenario: By mid-January, more than 850,200 people will catch the virus every day, which is more than 200% the peak reached last winter. 43,200 people would be hospitalized per day and 3,900 would die every day.
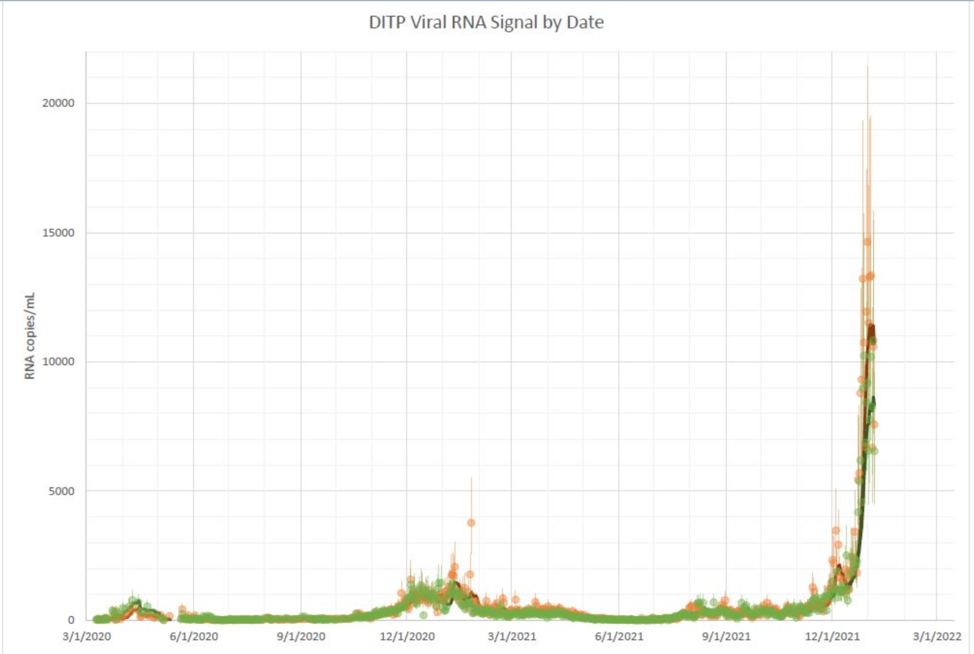
For a glimmer of hope, look at Boston’s sewage
Epidemiologist Dr. Katelyn Jetelina writes about how viral loads in wastewater can be a good indicator of how the virus is spreading. Notice that Boston’s sewage is showing a drop in viral load. OK, it is just a downward blip, but it is one of the few good signals we can point to today.
Jetelina says, “Once we reach that point, we still have a 3–4-week window for hospitalizations and deaths to peak. It will be a rough couple of weeks coming up.”
What is COVID decoupling and why does it matter?
Epidemiologists are chattering this week about something called decoupling, which refers to when COVID-19 cases don’t move in the same direction and rate as hospitalizations, intensive care unit admissions and deaths. As you know, the omicron variant is producing more positive tests than delta but has not produced as many deaths. That is decoupling.
Here is a link to a Financial Times graphic that tracks three data points in each state: cases, hospitalizations and ICU admissions. The green line on the graphic represents cases, blue is hospitalizations, and red is ICU patients. The dotted line on the graphic is the peak before omicron. You will notice something insightful: In a lot of states, we are passing delta-era peaks for hospitalizations, and certainly for new cases.
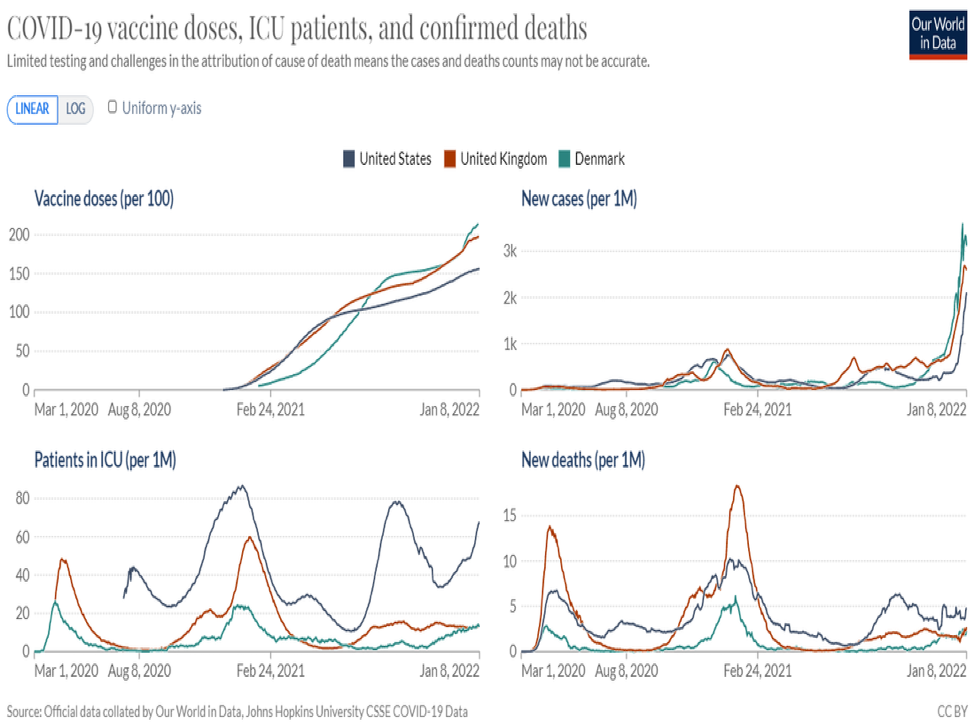
Jetelina cautions us against looking at places like South Africa, Great Britain or Denmark as an indication of when we can expect the worst of omicron to pass. For one thing, South Africa is in a summer season right now, while North Americans are inside for winter. She points out:
Nonetheless, what’s becoming clear is the decoupling phenomenon is less pronounced in the U.S. compared to other countries like Denmark and the U.K. There are clearly more cases in Denmark and the U.K. compared to the U.S. (see graphic below). However, the U.S. has many, many more patients in the ICU per capita. There are many reasons for this (like demographics, human behaviors, etc.), but the most glaring is that the U.S. started off at an already high rate (thanks to Delta) and has a lower vaccination (and specifically booster) rate.
When will there be a new COVID variant?

People wait in front of a pharmacy open on Sunday to get a COVID-19 test, in Paris, France, Sunday, Jan. 9, 2022. An unprecedented number of coronavirus infections is once again exposing the underfunding and shortcomings of public health care systems, even in developed parts of Europe. (AP Photo/Francois Mori)
Danny Altmann, professor of immunology at Imperial College London, told The Hill that until everyone everywhere has access to vaccines (and takes them), the next COVID-19 variant is “just around the corner.” And right on cue, a new variant has shown up in France.
It reportedly has 46 mutations from previously discovered variants.
Is this the next big thing? Who knows? But viruses mutate. The new virus that turned up in France has infected a dozen people but no more since it showed up in mid-November. The larger point is, there is more to come.
Many of the same epidemiologists who have breathed a sigh of relief over Omicron’s relatively low death rate are anticipating that the next lineage might be much worse.
Why is omicron less deadly than delta?
Every version of a virus acts differently, which is how they survive. But omicron, as The Daily Beast points out, “seems to infect the throat without necessarily descending to the lungs, where the potential for lasting or fatal damage is much, much higher.”
As we learned, omicron has experienced decoupling, which is when the overall case number does not produce more deaths. There is no way to predict if future variants will keep acting that way. A devastating scenario would be if there was a combination of omicron and delta, which would spread fast, end-run vaccines and attack the lungs. The Daily Beast talked with Edwin Michael, an epidemiologist at the Center for Global Health Infectious Disease Research at the University of South Florida:
When it comes to viral mutations, “extreme events can occur at a non-negligible rate, or probability, and can lead to large consequences,” Michael said. Imagine a lineage that’s as transmissible as Omicron but also attacks the lungs like Delta tends to do. Now imagine that this hypothetical lineage is even more adept than Omicron at evading the vaccines.
That would be the nightmare lineage. And it’s entirely conceivable it’s in our future. There are enough vaccine holdouts, such as the roughly 50 million Americans who say they’ll never get jabbed, that the SARS-CoV-2 pathogen should have ample opportunities for mutation.
“As long as we have unvaccinated people in this country—and across the globe—there is the potential for new and possibly more concerning viral variants to arise,” Aimee Bernard, a University of Colorado immunologist, told The Daily Beast.
Which leads to this sobering paragraph in The Daily Beast’s story, a paragraph that neither the president nor the CDC talks about:
A lineage much worse than Omicron could evolve at the same time that antibodies wane in billions of people all over the world. That’s why many experts believe the COVID vaccines will end up being annual or even semi-annual jabs. You’ll need a fourth jab, a fifth jab, a sixth jab, et cetera, forever.
A fourth shot, when it comes, would likely be late summer or early fall this year, according to Moderna CEO Stéphane Bancel.
Bancel said people who received their boosters last fall will likely have enough protection to get them through the winter, when new infections surge as people gather indoors to escape the cold.
However, Bancel said the efficacy of boosters will probably decline over the course of several months, similar to what happened with the first two doses. The Moderna chief was interviewed by Goldman Sachs during the investment bank’s health-care CEO conference.
“I will be surprised when we get that data in the coming weeks that it’s holding nicely over time — I would expect that it’s not going to hold great,” Bancel said, referring to the strength of the booster shots.
Congress is going to KN95 masks. Maybe you should, too.

A woman wearing KN95 medical mask. (Boumen Japet/Shutterstock)
Dan Diamond at The Washington Post got his hands on a Congressional memo:
Congress will start providing KN95 masks to House staff and lawmakers. Congress’ top doctor warned of “unprecedented infections at the Capitol.”
The memos says that each member of Congress’ office will get 40 KN95 masks per month. Until now, they have been getting less-protective surgical masks.
Norway’s military to issue used underwear because of supply chain problems
Norway’s NHK broadcasting reports that because of supply chain problems, Norway’s military is issuing used socks, bras and underwear to new conscripts. Norway has mandatory military service. When servicemembers complete their service, they now must turn in their undergarments to be reused.
IRS warns tax filings will be ‘an enormous challenge’ this year
The U.S. Treasury Department warns you not to count on getting your tax refund as fast as usual this year. Typically, the government starts the tax filing year with a million returns in backlog. Now the backlog is more than 6 million returns.
The IRS says the pandemic forced the closure of some processing centers and the Trump administration led a march to cut the staff by 25%.
We’ll be back tomorrow with a new edition of Covering COVID-19. Are you subscribed? Sign up here to get it delivered right to your inbox.